Development and implementation of a GafChromic EBT in-vivo personal dosimetry
|
|
|
- Stuart Cummings
- 6 years ago
- Views:
Transcription
1 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2008 Development and implementation of a GafChromic EBT in-vivo personal dosimetry Jacob R. Bugno Medical University of Ohio Follow this and additional works at: Recommended Citation Bugno, Jacob R., "Development and implementation of a GafChromic EBT in-vivo personal dosimetry" (2008). Theses and Dissertations This Thesis is brought to you for free and open access by The University of Toledo Digital Repository. It has been accepted for inclusion in Theses and Dissertations by an authorized administrator of The University of Toledo Digital Repository. For more information, please see the repository's About page.
2 Health Science Campus Examination Committee FINAL APPROVAL OF MASTER THESIS Master of Science in Biomedical Sciences Development and Implementation of a GafChromic EBT In-Vivo Personal Dosimetry System Submitted by: Jacob R. Bugno In partial fulfillment of the requirements for the degree of Master of Science in Biomedical Sciences Major Advisor: Ishmael Parsai, Ph.D. Academic Advisory Committee: John Feldman, Ph.D. Michael Dennis, Ph.D. Senior Associate Dean College of Graduate Studies Michael S. Bisesi, Ph.D. Date of Defense: July 23, 2008
3 Development and Implementation of a GafChromic EBT In-Vivo Dosimetry System Jacob R. Bugno University of Toledo 2008 Major Advisor: E. Ishmael Parsai, Ph.D.
4 Acknowledgment I want to take the time to first thank Dr. Ishmael Parsai for all that he has done for me. The education and opportunities provided me through his classes and more importantly clinic instruction has been helpful beyond measure. I would also like to thank Dr. John Feldmeier for the training and clinical instruction that he provided. Others that deserve thanks include Dave Pearson for help and instruction he provided throughout the clinic and the radiation therapists; (Ginger, Mary, Trisha, and Michelle) for assisting in the clinical placement of my films and being flexible with clinical time on the linac for research. ii
5 Table of Contents Acknowledgment... ii Table of Contents... iii Introduction...1 Literature...5 Materials...8 Methods...11 Results...29 Discussion...48 Conclusions...50 Summary...51 References...52 Abstract...56 iii
6 Introduction Since the beginning of the use of radiation to treat disease it has been of great importance to know how much radiation has been delivered. Knowing how much radiation has been delivered is generally calculated using a multitude of parameters. This can be accomplished many ways from a simple hand calculation to computer generated dose distributions created from complex algorithms running multiple iterations. Even with the use of highly accurate, complex modern treatment planning systems it is still sometimes useful to measure the dose delivered to the patient during a treatment. There can be areas of high dose or under dosage occurring especially when curved or irregular surfaces are being treated. In order to measure these dose differences and to make sure the patient is receiving the intended dose it is advantageous to measure dose during a treatment. Since we cannot place detectors inside the patient in areas that are intended to be treated we can instead place detectors on the patient s skin, the practice of this is known as in-vivo dosimetry. The process of in-vivo dosimetry is helpful because it can give us information about the dose delivered within the patient or on the patient s skin for any setup from a specific field up to an entire treatment or course of treatments. 1
7 In-vivo dosimetry can be done with a variety of detectors. The most common are photo stimulated thermoluminescence detectors (TLD), diodes, metal oxide semiconductor field effect transistors (MOSFET), and film. These detectors can share the common property of being relatively small so to not disturb or shield the radiation field from reaching its target. While each has its own benefits and drawbacks I will look further into film as an in vivo dosimeter. Originally radiographic film was used for in vivo dosimetry. The films consist of a transparent base coated with crystals of silver bromide. When the films are irradiated the silver bromide undergoes a reaction only in the area or irradiation. The silver bromide then undergoes chemical processing that converts it to metallic silver which is fixed to the film. Finally a wash removes the unaffected silver bromide (Khan, 2003). The remaining fixed metallic silver is what causes the film to be darkened. The intensity of the darkness is directly related to the amount of silver converted which is in turn related to the amount of radiation that passes through the film and is absorbed. Problems with the use of radiographic film used for in vivo dosimetry are encountered in the response of the film (i.e. the conversion of silver bromide into metallic silver) as well as in the processing of the film which is dependent on the tight control of chemical activity, solution temperature, and processing time. The inconsistencies in both of these aspects of radiation detection result in radiographic film to not be the best choice in absolute dosimetry measurements. 2
8 Even though convention radiographic film proved to not be the best choice for absolute dosimetry measurements, the development of commercially viable medically usable radiochromic film in the late 1960 s has made film an attractive and convenient tool. Radiochromic films differ from conventional radiographic films in the method that radiation produces coloration. Radiographic films are made up of layers; a base of a polyester material is used as well as a layer of sensitive material which reacts with ionizing radiation. Films can have multiple layers so that there may be a number of sensitive layers within one film. These layers tend to be on the order of microns thick so that even though a film may contain multiple layers it is still the thickness of what one would expect for a film. The sensitive layers are made from an organic conductive polymer named polydiacetylene. This polymer is dispersed by coating a flexible polyester film base. During irradiation there occurs a polymerization reaction initiated by the ionizing radiation, resulting in homogeneous color change. The films are colorless before irradiation, and then turning progressively blue upon exposure. One of the key benefits of this type of film is that the radiation-induced color change is formed without thermal, optical, or chemical development and the image is stable (Niroomand-Rad et al., 1998) 3
9 As with radiographic films, radiochromic films are measured using a device that determines optical density. The most common tools used to measure films are flatbed scanners, transmission scanners, or densitometer. All three of these machines measure optical density which is defined by the following formula, where the optical density (OD) is equal to the log of the ratio of light transmitter through a film (I t ) to light present with no film to block it (I o ). I OD = log o It As the film is darkened by receiving more radiation or higher dose the optical density increases. By delivering known amounts of radiation to films and then measuring their optical densities a graph can be created to establish the link between the films polymerization due to irradiation and delivered dose. With such a graph, subsequent films of unknown dose can be measured to find their optical density and then plotted to determine corresponding dose. Commercially available radiochromic film has been primarily produced in and marketed under the name Gafchromic film by the company international specialty products. They have produced many variations of film each with a different composition. Their newest model named EBT is what I selected to use for creation of an in vivo dosimetry system. You can see the differences in composition in the following image provided by Devic et al.,
10 Radiochromic Film Composition Fig 1: Selection of available radiochromic films as well as their design. Literature There has much interest in the new EBT radiochromic film from the radiation oncology community. As a result of this there has already been extensive novel research on the characteristics and responses of the film to different scanning and irradiation techniques. One of the first aspects of the new film to be reviewed was the energy dependence of the film. It was found in studies by Butson et al. (2006) to not exceed a 10% variation over the energy range of 50 KVp to 10 MVp photons. Other work by International Specialty Products (2006a) shows there to be little energy dependence throughout the kilo voltage to megavoltage photon range, as well as the megavoltage electron range as shown in Figure 2. 5
11 Multiple Energy EBT sensitometric data Fig 2: International Specialty Products chart of multiple energy OD vs. Dose In addition to energy dependency much work was done on post irradiation optical density correspondence. As shown by Cheung et al (2005) the Gafchromic EBT film has an approximate 6% to 9% increase in post irradiation optical density within the first 12 hours of irradiation. He also notes that the optical density growth levels out to 1% within the first 6 hours. Post Irradiation Film Response Fig 3: Cheung et al (2005) post irradiation film coloration change as a function of time 6
12 However the post irradiation changes cited by Cheung et al, (2005) does not match results from International Specialty Products (2006a) stating that EBT film optical density change is <10% total and is effectively complete in less than 2 hours. Fig 4: ISP (2006a) post irradiation film coloration change as a function of time One thing that was agreed upon is that calibration films must be read out at the same time post irradiation to make sure they are all in the same response period and thus further enhance the accuracy. Another aspect of the film that was studied was its absorption spetrum. It was shown as seen in Figure 5, by (Rink et al., 2005 and International Specialty Products 2006a) that the wavelength of maximum change in absorbance occurs at 636 nm 7
13 Change in light absorbance vs. wavelength Fig 5: Change in absorbance of EBT film over a range of wavelengths before, immediately after, and at two time points post exposure (Rink et al., 2005). Finally, clinical studies similar to mine conducted by Devic et al. (2006) show that EBT skin measurements based off of a single films piece would overestimate the dose by approximately five percent. This high of a percentage is would be outside of a normal clinical tolerance however as you will see, the skin dose expected from the treatment planning system are not accurate to begin with. Materials Materials used to conduct this research include the Vidar VXR-16 Dosimetry Pro transmission film scanner used to scan the chromic film and determine optical density and scanner analog to digital values as seen in the following picture. 8
14 Vidar VXR-16 Fig 6: Vidar VXR-16 Dosimetry Pro scanner used to scan films into analysis software In addition to the Vidar scanner, Microsoft Excel was used extensively especially in data analysis and creation of graphs, tables, and figures. Other software used is RIT113 by Radiological Imaging Technologies Inc. This software is an image analysis package allowing interface with the Vidar scanner to save, edit, crop and measure images. It was used to read all of the film and provide the necessary data for calibration of the chromic film. Measurements were taken with Gafchromic EBT film on an Elekta Precise SL-25 linear accelerator. Films were irritated with multiple energies of, 6, 10, and 18 MV photons and 6, 9, and 12 MeV electrons. Measurements were taken with a phantom of solid water blocks as seen below. 9
15 Elekta SL-25 Fig 7: Elekta Precise SL-25 linac with solid poly phantom, setup to 100cm SSD with film placed at a depth of five cm. They were also placed clinically to take surface and maximum dose measurements. These doses were found from the patient s treatment plan created on an ADAC Pinnacle treatment planning system. Additional dosimetric data was also used from the second check calculation program RadCalc. 10
16 Method To begin creating a chromic film in-vivo dosimetry system one has to create calibration curves that allow the correlation of optical density to dose. Before these calibration curves were made I had to establish what range of doses I would want the system and calibration curves to be able to measure. Instead of just arbitrarily selecting a dose range I looked to the past to help me select a range that would cover the majority of the doses seen in the clinic. To do this I went to the database of RadCalc diode measurements from previous years. RadCalc is used to double check dosimetry calculations as well as provide us expected diode measurements for use with our MOSFET diode system. Every patient is sent through RadCalc so sampling from the database would result in a truly random and wide range of treatments and prescriptions. RadCalc diode sheets are generated for every patient that has a treatment utilizing wedges; it is these patients that I sampled for my dose range. Diode sheets contain D max doses which were then statistically analyzed to determine the dose range. D max doses were used because they represent the maximum dose that a singe field could generate; therefore if the system is calibrated high enough to read D max it will be able to read lower doses. The doses that were used in establishing my dose range is seen below in Table i. 11
17 2005 and 2006 RadCalc D max Doses Table i These doses were entered into Microsoft Excel where statistical analysis could be preformed. Statistical analysis was based on the Gaussian distribution (Knoll, 2000). The first step in the analysis was to determine the mean value with the following formula where µ is the mean, n the total number of readings, and x i is each individual reading: 1 n xi n i= 1 μ = Once the mean was found I was able to find the standard deviation of the data set with the following equation. 1 n i ( x μ ) 2 σ = n i= 1 12
18 With both the standard deviation and the mean found I was able to use produce a Gaussian distribution to graphically show the probability of observing any given D max dose. The probability density function shown below was used and is of course a function dependent on x, the individual D max dose, µ the mean, and σ the standard deviation. 1 2 x μ 1 2 σ f( x; μσ, ) = e σ 2π When the previous function is graphed, the results can be seen in Figure Revised Gaussian Distribution of RadCal Dmax Doses (high dose readings removed) RadCalc Dmax Dose Fig 8: Gaussian distribution of the RadCalc D max doses found in table i 13
19 With the Gaussian distribution established I then proceeded to determine the range of doses I would use to calibrate the film to. This was done using what is known as a confidence interval or the probability of occurrence of given deviations. Tabulated values for the probability of occurrence are provided (Knoll, 2000) and give the probability of a random dose will show a normalized deviation less then the value from the Gaussian distribution created. I chose to use a probability of occurrence of 95% which means that 95% of all the doses will fall into my range which is 1.96 the value of the standard deviation. With the previously stated mean and standard deviation formulas I determined the following range. μ = σ = 44.6 Lower Value = μ 1.96σ = 36.0 Upper Value = μ+ 1.96σ = To help visualize what this means I have created Figure 10, where the shaded region under the Gaussian distribution starting at a dose of 36 and ending at a dose of represents 95% of doses. As you can see there will be a small 2.5% possibility that a dose will be lower or higher then my range. 14
20 0.01 Revised Gaussian Distribution of RadCalc Dmax Doses (high dose readings removed) RadCalc Dmax Dose Fig 10: Graphical representation of the 95% probability of occurrence within the Gaussian distribution. With a dose range of established I created a list of each specific dose I would create a calibration film at. The RIT software module I used to create the calibration films required a minimum of 13 data points so I decided to add a few and have 25 calibration doses for regular measurements and another 25 for skin doses measurements. I set this range with a simple linear distribution as seen in the following figures. 15
21 Linear Selection of Doses used for calibration 250 Calibration Doses 40 Skin Calibration Doses Dose 100 Dose Fig 11: Left Calibration doses selected linearly, Right Skin calibration doses selected linearly. The actual calibration doses can be seen in the following table, Table ii. Calibration Doses (cgy) Surface Calibration Doses (cgy) Table ii: List of Calibration doses including Surface/Skin 16
22 Since I intended to use this dosimetry system to measure not only D max doses but more importantly skin or surface doses I found it important to also create a lower dose set of calibration points. With lower dose data points on the calibration curve it would allow for greater accuracy when measuring doses that would be below 36 cgy. Since it was already shown in earlier studies (Parsai, 2006) that the surface dose is on the order of 10% - 20% of the D max dose and the highest D max dose in our calibration was 211 cgy I decided to also setup calibration points from 0 to 36 in a linear distribution of 25 data points as shown in Table ii and Figure 11. With the dose range selected work began on the setup of the measurement system. As stated before, the films optical density is measured with the Vidar VXR-16 film scanner and analysis software RIT113. In order to achieve this, the optical density (OD) of the chromic film must be correlated to the scanners A/D value. This was done using a baseline film to create an OD calibration curve also known as an OD Step wedge calibration curve. The reason it is called an optical density step wedge is because the film is striated into multiple steps of different known optical density. During the scanning process the film is passed through the Vidar VXR-16 scanner where a white light source is transmitted through the film and onto a solid state detector (CCD). The detector varies the voltage it outputs depending on the intensity of the light that falls on it, which is directly related to the optical density of the film. The sensor itself is an analog device and its signal must be converted into a digital signal for analysis, this is done buy an analog to digital converted and the resulting signal is known as the scanner A/D value. 17
23 By scanning the step wedge film with known optical densities I am able to correlate the scanner A/D value to a given optical density, thus creating an OD Step wedge calibration curve as shown in Figure OD Step Wedge Calibration OD Scanner A/D Fig 12: Optical density step wedge calibration curve With the Step wedge calibration file I am able to determine scanner A/D values for films of different unknown optical density. This will be used by the RIT113 software to determine scanner A/D values for chromic films receiving different doses and thus create my chromic film calibration curves. 18
24 With the scanner and analysis software setup I began creating the irradiation setup and associated excel file for calculation of monitor units and dose delivered. I began with basic SSD method calculations to determine the monitor units needed to achieve the desired doses which were determined in my statistical analysis and listed previously in Table ii. Following (Kahn, F.M, 2003) I adopted the following formula for determining the monitor units for irradiation of my films. TD 100 MU = K (% DD ) S ( r ) S ( r ) ( SSD factor ) c c p Where MU is the number of monitor units, TD is target dose, %DD is the percent depth dose at a given depth, S c (r c ) is the collimator scatter factor, S p (r) is the phantom scatter factor, K is the output which is assumed to be 1 cgy per MU, and finally the SSD factor. This formula can be simplified using the following formulas; the first combines the collimator and phantom scatter factors into one factor which we call an output factor or field size factor, calculated by taking a ratio of our standard 10x10 cm square field to other field sizes. Scp, () r = Sc() r Sp() r The SSD Factor is explained by the following formula: SSD SCD factor = SSD + t0 2 19
25 Where SCD is the source to calibration point distance, SSD is the source to surface distance, and t 0 is the reference depth. Since I performed all of my film irradiations at an SSD of 100cm the SSD Factor will always be 1.0 because the SCD and SSD + t o will be equal which you can see with a quick calculation using the formula above. With all of the formulas stated above I created a excel sheet to calculate MU s for each of the doses that the film would be irradiated at. Depth dose as well as in-plane and cross-plane profile scans were performed using the Wellhoffer blue water scanning phantom and Omni-pro acceptance scanning software. These depth dose curves were then exported into Excel files and can be seen below. Elekta SL-25 Annual PDD and Profiles 120 Photon % DD 120 Electron Percent Depth Dose % DD X 10X 18X % DD e 9e 12e 15e 18e 22e Depth (cm) Depth (cm) Photon Inline Profiles at 5.0 cm Depth 120 Electron Inplane Profile e 6e 9e 12e 18e 22e Position (cm) 10X 6X 18X Position (cm) Fig 13: Photon and Electron depth dose curves and profiles. 20
26 The following table is a copy of one of the Excel calculation pages used to determine MU s to deliver to achieve the desired dose to the film itself. Sample MU calculation worksheet for film irradiation TD 100 MU = K (% DD ) S ( r ) ( SSD factor ) cp, Dose (cgy) 5cm Sc,p (20x20) K SSD factor MU Table iii: Excel data for calculating monitor units to irradiate film to given dose. 21
27 Setup for the irradiation of the calibration films for photon energies was done at 100 cm SSD, with a field size of 20 x 20 cm square field and the film at depth of 5.0 cm in solid water equivalent poly phantom corresponding to other calibration setups (Niroomand-Rad et al., 1998). Electron setup parameters were identical with the exception that the films were placed at a depth of 2.0 cm for energies 6 MeV and 9 MeV and 2.6 cm for 12 MeV. The %DD at depth as well as the S c,p (r) for 20 x 20 cm fields were determined from measurements made and depth dose data. Setup of the irradiation can be seen in the following photographs. Photon irradiation setup Fig 14: Photon irradiation setup, 100cm SSD, 20x20cm field size. 22
28 Electron irradiation setup Fig 15: Electron irradiation setup, 100cm SSD, D max depth, 20x20cm field size. With the monitor units calculated and the irradiation setup decided upon I began preparing the chromic film for irradiation. I first oriented all of the pieces of film in the same direction since we already learned that orientation during scanning affects the results. The films were all marked with a permanent marker on the top right corner of the film. This allowed the same orientation to easily be reproduced. The films were then cut into 2.0 cm by 2.5 cm rectangles. Each smaller piece of film was also labeled to continue the orientation system with markings on the top right corners. The size of the film pieces allowed for an area to be used to label the films in addition to its orientation marking as well as a size large enough to be manageable without tweezers but not so big as to be cumbersome. This size also allowed for a larger selection of regions of interest so that multiple locations on the film or a larger area could be averaged for a single reading. 23
29 When I began irradiation of the film pieces they were placed in the phantom at the center of the beam. The orientation of the films during irradiation does not matter so all I was concerned with was placing them at the central axis of the beam. I would then leave the vault and irradiate the piece of film with the monitor units calculated for the given dose. I would then label the film with the dose it received and place it into an envelope containing all fifty films for a specific energy. I would then irradiate the next fifty films for the next energy and so on until all the energies had there calibration films irradiated to the doses established in table ii. With the films irradiated I could begin analyzing the results and constructing calibration curves. All of the films were stored for a minimum of two hours before they were scanned to allow for the polymerization processes to fully occur otherwise post irradiation scanning would deliver different results as shown previously in Figure 4. The films were scanned in the Vidar VXR-16 utilizing the RIT311 scanning software to perform analysis. All of the scanning was done in a custom made template to hold the films as shown in Figure 17 below detailing the scanning instructions. The template was cut from a blank film and allowed each individual piece of chromic film to be taped in an opening. This created an adequate holder for films that both allowed for unobstructed light transmission during scanning as well as not blocking areas of the film other then the corners or edges. 24
30 Once films were placed into the template and loaded into the Vidar scanner the RIT311 software was loaded and scanning parameters were selected. All of the scans were done at a resolution of 178, meaning that there are 7.53 pixels per micron. The film size of 14x17 was selected from the options and scanning commenced. Other parameters that are not changed include the filter method and size, which should default to a median filter of 5x5 size. This means that data will be smoothed by ordering the pixel values of a 5x5 square of pixels and then replacing the center pixel with the average while still preserving the edges, this method is default and strongly recommended by the RIT311 (Radiological Imaging Technologies Inc, 2006). After the scan the perpendicular dose calibration module was used to determine the A/D value from the films. First the optical density step wedge file was selected then with a region of interest (ROI) of 0.75 x 0.75 cm selected I would determine the A/D value and enter it into a custom excel sheet where calibration curves were created. In addition to irradiating and scanning all of the films for creating calibration curves, I also irradiated films for statistical analysis. I irradiated three batches of 25 films for high dose, medium dose, and low dose statistical analysis. For the high dose films, each 25 films were irradiated to a dose of 139 cgy with energy of 10 MV according to the standard irradiation procedure described previously. The medium and low dose films were irradiated with a 10 MV beam as well, to doses of 35 and 13 cgy respectively. All films were scanned according to the standard scanning parameters and analyzed in Microsoft Excel to examine reproducibility. 25
31 Surface dose films were also irradiated. They consisted of five films at energies of 6 MV, 18 MV, 6 MeV, and 12 MeV. The films were irradiated to different doses as well as at different field sizes. All were irradiated on top of a solid water poly phantom. They were all setup with a 100 cm SSD and placed in the center axis of the field. They were also scanned in a standard manner with analysis probing qualities of the film when used without buildup for measuring skin doses. Blank films were placed clinically to perform real world testing. Patients were selected at random with the majority being treated for breast, prostate, and head and neck cancers. Both conventional and intensity modulated radiation therapy (IMRT) was used to treat the patients. The films were placed by the radiation therapists at the center axis of the field. A combination of plain skin readings as well as buildup covered readings intended to correspond to D max values were taken. Buildup used consisted of the poly buildup caps used clinically for the MOSFET diode buildup. Some films were irradiated by single fields while others were left on the patient while all of their fields were treated. Images below show the location of some of the films during clinical measurements. Clinical Film Locations Fig 16: Locations of films noted by blue dot during clinical film irradiation. 26
32 Finally a set of scanning instructions were created that diagram and explain the proper scanning procedures for the films. The steps in the instructions are the exact steps used to scan all of the films used in creation of the calibration curves as well as the testing of the patient films, statistical analysis films, and surface dose films. The instructions are shown on the following page. Film Scanning Instructions Fig 17: First two pages of the film scanning instructions 27
33 Film Scanning Instructions continued Fig 18: Scanning and reading instructions continued 28
34 Results The first results that were obtained were the chromic film calibration curves. To begin I scanned all of the films and recorded the dose they were irradiated to along with the scanned analog-to-digital (A/D) value. Then utilizing an Excel spreadsheet I plotted the dose vs. A/D value to obtain a graph of the resulting calibration curve. The following graphs show the calibration curves for the 6 MV photons. 6 MV calibration data 250 6X Dose / AD Value Correlation Dose (cgy) E E E E E E+04 A/D Value Fig 19: 6 MV calibration curve 29
35 As you can see there is a trend in the data that as the dose decreases the A/D value increases. This is just as I suspected because the lower dose results in less polymerization of the films and a subsequent lighter color allowing more light to pass through the films during scanning. To model this trend and have meaningful data to work with I fitted the data to a polynomial equation of the third power because it achieved the best possible correlation coefficient. You can see in on the same graph that with the addition of the trendline and equation that the calibration data now can be used to determined dose with a simple calculation. 6 MV calibration data with fitted trendline 250 6X Dose / AD Value Correlation y = -4E-12x 3 + 7E-07x x R 2 = Dose (cgy) E E E E E E+04 A/D Value Fig 20: 6 MV calibration curve with fitted trendline and equation The reason that a polynomial trendline was used is that it achieved the best possible fit. The correlation coefficient, which is a measure of how close the estimated trendline values are to the actual values, where 1.0 is a perfect fit had an average of around
36 Once I began comparing calibration curves of multiple energies I initially came across an unknown problem. Since I already expected the data to be energy independent I was puzzled by the discrepancy between the 6 MV and 10 MV/18 MV data when I first compared them. The following graph is what I initially had as my photon comparison. 6 MV, 10 MV, 18 MV Calibration Curves 250 Photon Energy Dose / AD Value Correlation 6x 10x 18x 200 Poly. (6x) Poly. (10x) Poly. (18x) 150 Dose (cgy) A/D Value Fig 21: 6 MV, 10 MV, 18 MV calibration curves. 6 MV curve off due to scanning orientation. As you can see there is roughly a 400 value difference in A/D values between the 18 MV and 10 MV energies to the 6 MV for a given dose. This discrepancy could not be explained even after rescanning the films so I irradiated a new batch of films and scanned them. The new batches of 6 MV films were right in line with the 10 MV and 18 MV Deleted: 6x Deleted: 6x curves as can be seen in the graph of all the photon calibration curves shown below. 31
37 250 Photon Energy Dose / AD Value Correlation 10X 18X 6x Poly. (10X) Poly. (18X) Poly. (6x) Dose (cgy) E E E E E E+04 A/D Value Fig 22: photon calibration curve after correction of 6 MV Deleted: 6x The anomaly that was found in the first batch of 6 MV chromic films was at first puzzling. It was not until later that I discovered why the data was shifted. I had scanned the films that correspond to that shifted 6 MV data in a different orientation then the rest Deleted: 6x Deleted: 6x of the films. This demonstrated the importance of marking the films with the dot in the upper right hand corner and scanning then exactly according to my scanning instructions. With the photon energy data analyzed I processed the electron data. The electron data showed no apparent anomalies and can be seen in the following graph. 32
38 250 Electron Energy Dose / AD Value Correlation 6e 9e 12e Poly. (6e) Poly. (9e) Poly. (12e) Dose (cgy) E E E E E E+04 A/D Value Fig 23: Electron Calibration Curve A compilation of all of the energies together is seen below. 250 Multiple Energy Dose / AD Value Correlation 10X 18X 6e 9e 12e 6x Poly. (10X) Poly. (18X) Poly. (6e) Poly. (9e) Poly. (12e) Poly. (6x) Dose (cgy) E E E E E E+04 A/D Value Fig 24: All energies calibration curve 33
39 With all of the energies completed and trend lines added I began to compute an overall equation for determining dose from A/D value that could then be used clinically. As you can see in the previous graph there are slight differences in the trend lines of each of the energies. I decided to compute one formula to use for clinical practice. The formula is an average of all energies of the trend line equations. Each of the trend line equations is listed below as well as the computed average which was done by averaging each order of the polynomial and then recombining them again. ( ) ( ) ( ) ( ) ( ) ( ) ( ADvalue ) ( - ADvalue ) ( ADvalue) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) x Dose = ADvalue ADvalue ADvalue x Dose = ADvalue ADvalue ADvalue x Dose = e Dose = ADvalue ADvalue ADvalue e Dose = ADvalue ADvalue ADvalue e Dose = ADvalue ADvalue ADvalue Average Dose = ADvalue ADvalue ADvalue With the creation of a universal formula to determine dose I then focused on statistical analysis of the irradiated films and their resulting scanned A/D values. This was done by analyzing the high-medium-low dose films that were all irradiated to the same doses of 139 cgy, 35 cgy, and 13 cgy respectively. The following table is the resulting A/D values for the three doses along with a graphical representation of the data. 34
40 Statistical Analysis Data A/D Value Film # High (139 cgy) Med (35 cgy) Low (13 cgy) Table iv: Film data taken to run statistical analysis on 35
41 50000 Graphical Representation of Table iii Statistical Film Analysis A/D Value High (139 cgy) Med (35 cgy) 5000 Low (13 cgy) Film Number Fig 25: statistical data graphed The results of this test show that my method of analysis produces a constant reading for a given dose. This data was analyzed further by determining the standard deviation for each of the different data sets using the standard deviation formula from before. 1 n i ( x μ ) 2 σ = n i= 1 The following are the calculated standard deviations. Standard Deviation of Statistical Data Table iii Data Set Standard Deviation Low Dose (13 cgy) Medium Dose (35 cgy) High Dose (139 cgy) Average
42 Since the standard deviation of the A/D values would be used to determine the error range of the dose calculation the average of all of the batches was taken and used for further calculations. Using the already determined dose formula from the calibration curves I added the standard deviation from the statistical analysis to find the final dose calculation formula with error accounted for. By using an error range of plus or minus one standard deviation I established that the standard deviation of the A/D values does not directly correlate to a meaningful dose. For example using the calibration curve dose formula an A/D value of 298 would equal a dose of 1,095 cgy. Obviously a dose cannot be plus or minus 1,095 cgy. In addition to this the error range of dose changes with the chromic films A/D value. It can be larger or smaller depending on the location that the films A/D value lies on the calibration curve. The reason for this is because the calibration curve is not linear and hence the slope of the curve changes resulting in changes in error ranges. The graph below demonstrates this principle. A hypothetical film is scanned and the resulting A/D value falls on the calibration curve plotted as the red dot. The standard deviation in A/D values of 298 is applied to the films A/D value and the resulting dose and error range are found. 37
43 Error Analysis of Film reading Dose error range A/D Value A/D Value Fig 26: graphical representation of calibration curve slope effect on error range As you can see as the slope of the curve decreases the resulting dose range corresponding to the ± 298 A/D value also decreases. In order to account for this I created two formulas, one for the dose which remains the same as stated previously and another to calculate the error. The one to calculate the error is just an extension of the formula found before from the calibration curves. Again the formula to determine dose calculated from the calibration curves is ( ) + ( ) ( ) + ( ) Dose = A/D Value A/D Value A/D Value You can see that dose is only a function of A/D value so for simplification I will express the formulas in terms of this variable, so the previous formula can be written as: Dose(A/D Value) To find the error I then took the average of the addition and subtraction of the standard deviation dose from the dose of the A/D value of the film. 38
44 Error(A/D Value) = [ Dose(A/D Value + 298) - Dose(A/D Value) ] + [ Dose(A/D Value) - Dose(A/D Value - 298) ] 2 Each formula is then brought together to create the final dose determination formula. Dose(A/D Value) ± Error(A/D Value) With all of the data collected an analyzed I compiled it into a clinical dose form that is based in excel allowing the user to simply input the scanned A/D value, the formulas above are then used to calculate the dose the film received as well as the potential error in that dose. This clinical dose form also contains data fields for patient, scanning, and placement information and can be seen in Fig
45 Clinical Film Calculation and Report Sheet RadioChromic Film Dosimetry Report University of Toledo Medical Center Department of Radiation Oncology Patient Name: Treatment Site: Field Name(s): ID Number: Diagonisis: Field ID(s): Film ID: Irradiaton Date/Time: / Scan Date/Time: / (Scan Time > 2:00 hours post irradiation) ROI Size: A/D Value = ± ( ) + ( ) ( ) + ( ) Dose = A/D Value A/D Value A/D Value Dose (cgy) = 1112 ± 17 m Placement Notes: Calculated By: Physician Signature: Date: Date: University of Toledo Medical Center Dept. of Radiation Oncology Medical Physics / Dosimetry Fig 27: Excel worksheet used for clinical dose calculation and reporting 40
46 Now that the dose formula was completely established I began analyzing the clinical data acquired by placing the pieces of chromic film on actual patients undergoing treatment. The placement of the films varied in terms of location as well as treatment type and energy. Table v below summarizes the films measurement type, site, setup, energy, and the expected dose. Clinical Film Placement/Parameter Summary Film # Type Site Setup Energy Expected Dose 1 Dmax Breast - Ctrl Pt. Calc Pt. w/ buildup 6 MV Skin Breast - Ctrl Pt. Calc Pt. w/o buildup for both beams 6 MV Skin Pelvis - 4 fld Calc Pt. w/o buildup for all beams AP/Lats 18 MV, PA 6MV Skin IMRT H&N Beam Iso w/o buildup all beams 6 MV Skin IMRT H&N Beam Iso w/o buildup all beams 6 MV Dmax IMRT H&N Beam Iso w/ buildup 6 MV Skin IMRT H&N Beam Iso w/o buildup all beams 6 MV Skin IMRT H&N Beam Iso w/o buildup all beams 6 MV Dmax Pelvis - 4 fld Rt Calc Pt. w/ buildup (3cm) 18 MV Skin IMRT H&N Beam Iso w/o buildup all beams 6 MV Skin Breast - Ctrl Pt. Calc Pt. w/o buildup all beams 6 MV Dmax Breast - Ctrl Pt. Calc Pt. w/ buildup 6 MV Dmax Breast - Ctrl Pt. Calc Pt. w/ buildup 6 MV Skin Breast - Ctrl Pt. Calc Pt. w/o buildup for both beams 6 MV Skin Pelvis - 2fld Iso w/o buildup all beams 18 MV 68.3 Table v: clinical film placement parameters Buildup was achieved with either the MOSFET diode buildup caps or in the cases of high energy a custom built bolus buildup cap. The films were all placed along the central axis of their respected field and measured according to the previously defined scanning procedures. 41
47 The expected doses were found in two different methods depending on the type of reading that was taken. D max expected doses were found using RadCalc. The patients plan was imported into Radcalc then a diode calculation sheet was generated by Radcalc. The results are the calculated D max dose value for each beam on the center axis. Skin expected doses were found through the ADAC treatment planning system. The films were placed at central-axis of a beam and then left there the whole treatment. In order to find the dose to the skin at this point I copied the beam they were placed under in ADAC. I then created a new dose tracking point and placed the copied beam to this new point, in order to set the dose tracking point to the skin surface I then set the SSD of the copied beam to 100, effectively placing the point on the patient s skin surface. The dose to this point was then taken to be the expected skin dose. This technique is illustrated in the following diagrams. ADAC Skin Dose Measurment Setup Fig 28: Technique used to determine skin doses. Treatment field (blue) and corresponding calc point (red) are copied. New calc point (blue) is then set to skin distance by setting copied beam (red) to 100 SSD. 42
48 With each of the patient films collected the scanning began. In addition to scanning with the standard 0.75 x 0.75 region of interest (ROI) I also scanned twice more with an ROI of 0.5 x 0.5 and 0.2 x 0.2. Each of the ROI s was centered in on the film. This not only allowed me to compare the chromic film results to the expected ADAC and RadCalc doses but examine the results of what happens when region of interest was used to determine the A/D value. The following chart examines the difference between scanning at different ROI s. It lists the doses without considering error and compares the three results with the absolute difference between the lowest and higest dose. Dose Comparison of ROI size 0.75 x 0.75 ROI Dose 0.5 x 0.5 ROI Dose 0.2 x 0.2 ROI Dose Min Value Max Value Max Dose Difference Table vi: Dose difference for same films, different ROI sizes As you can see the maximum difference in dose between the different ROI s is very low on the order of one to two cgy with an average of This result is important because it shows that the ROI used to determine the A/D value is not of much consequence and thus allows for more options with the films. 43
49 When comparing the expected doses to the measured doses the results. I sorted the data by first weather the type of measurement was D max or skin dose; second I sorted by the percent error of the measured dose. As you can see there is a large percent error between the measured and the expected doses in the skin dose measurements. The D max measurements resulted in percent errors ranging from 1.7% to 9.3%. Clinical Film dose compared to Expected dose Film # Type of Measurment Expected Dose Measured Dose Percent Error 12 Dmax ± % ± 2.8% 13 Dmax ± % ± 2.9% 9 Dmax ± % ± 3.8% 6 Dmax ± % ± 14.2% 1 Dmax ± % ± 3.1% 11 Skin ± % ± 3.8% 3 Skin ± % ± 4.6% 15 Skin ± % ± 4.7% 4 Skin ± % ± 5.6% 5 Skin ± % ± 5.6% 10 Skin ± % ± 8.7% 7 Skin ± % ± 5.9% 8 Skin ± % ± 5.9% 14 Skin ± % ± 31.2% 2 Skin ± % ± 34.1% Table vii: Clinical films sorted by type of measurement with corresponding expected dose from TPS and measured dose with percentage difference It is obvious from the results that the chromic film readings are not matching the expected readings from ADAC TPS for the skin measurements. This indicates one of two possibilities. Either the films are not accurate at detecting the skin dose or the ADAC TPS is not accurate in its calculations of expected dose when the dose point is placed on the skin. 44
50 Seeing how the dose calculation algorithm used in ADAC is based off of percent depth dose measurements taken with a standard farmer chamber, which is known from previous research (Parsai, E.I. et al., 2006) to not be as much as 30% higher in the buildup region as other measurement devices, I took more surface films on a solid phantom to compare against more accurate estimated skin doses. As described previously I took surface dose films on a solid water phantom with 100cm SSD and a variety of energies and field sizes. The chart below are my resulting A/D values, measured doses and calculated D max doses with corresponding surface %DD. Phantom Surface Dose Film Test Resutls Film # Energy FS (side of square) MU's A/D Value Dose (cgy) Calculated Dmax Dose % DD at Surface 1 6x % 2 6x % 3 6x % 4 6x % 5 6x % 6 18x % 7 18x % 8 18x % 9 18x % 10 18x % 11 6e % 12 6e % 13 6e % 14 6e % 15 6e % 16 12e % 17 12e % 18 12e % 19 12e % 20 12e % Table viii: Results of films placed on a phantom surface along with calculated percent depth dose at the surface from the film data 45
A SYSTEM OF DOSIMETRIC CALCULATIONS
 A SYSTEM OF DOSIMETRIC CALCULATIONS INTRODUCTION Dose calculation based on PDD and TAR have Limitations The dependence of PDD on SSD Not suitable for isocentric techniques TAR and SAR does not depend on
A SYSTEM OF DOSIMETRIC CALCULATIONS INTRODUCTION Dose calculation based on PDD and TAR have Limitations The dependence of PDD on SSD Not suitable for isocentric techniques TAR and SAR does not depend on
A DOSIMETRIC MODEL FOR SMALL-FIELD ELECTRON RADIATION THERAPY A CREATIVE PROJECT (3 SEMESTER HOURS) SUBMITTED TO THE GRADUATE SCHOOL
 A DOSIMETRIC MODEL FOR SMALL-FIELD ELECTRON RADIATION THERAPY A CREATIVE PROJECT (3 SEMESTER HOURS) SUBMITTED TO THE GRADUATE SCHOOL IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE MASTER OF
A DOSIMETRIC MODEL FOR SMALL-FIELD ELECTRON RADIATION THERAPY A CREATIVE PROJECT (3 SEMESTER HOURS) SUBMITTED TO THE GRADUATE SCHOOL IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE MASTER OF
Basic Radiation Oncology Physics
 Basic Radiation Oncology Physics T. Ganesh, Ph.D., DABR Chief Medical Physicist Fortis Memorial Research Institute Gurgaon Acknowledgment: I gratefully acknowledge the IAEA resources of teaching slides
Basic Radiation Oncology Physics T. Ganesh, Ph.D., DABR Chief Medical Physicist Fortis Memorial Research Institute Gurgaon Acknowledgment: I gratefully acknowledge the IAEA resources of teaching slides
Machine and Physics Data Guide
 WWW..COM Machine and Physics Data Guide STANDARD IMAGING, INC. 3120 Deming Way Middleton, WI 53562-1461 May / 2008 2008 Standard Imaging, Inc. TEL 800.261.4446 TEL 608.831.0025 FAX 608.831.2202 www.standardimaging.com
WWW..COM Machine and Physics Data Guide STANDARD IMAGING, INC. 3120 Deming Way Middleton, WI 53562-1461 May / 2008 2008 Standard Imaging, Inc. TEL 800.261.4446 TEL 608.831.0025 FAX 608.831.2202 www.standardimaging.com
GafChromic Protocol Multi-Channel Film Dosimetry + Gamma Map Analysis
 GafChromic Protocol Multi-Channel Film Dosimetry + Gamma Map Analysis Micke A. Ashland Inc. Advanced Materials Ashland proprietary patented technology GafChromic Film for Dose Measurement Radiotherapy
GafChromic Protocol Multi-Channel Film Dosimetry + Gamma Map Analysis Micke A. Ashland Inc. Advanced Materials Ashland proprietary patented technology GafChromic Film for Dose Measurement Radiotherapy
Quick Reference Datasheet For All RIT113 Packages
 Quick Reference Datasheet For All RIT113 Packages For Rotational Therapies, IMRT & TG142 Highlights and selected product information only. A complete TG142 brochure is available. For more information on
Quick Reference Datasheet For All RIT113 Packages For Rotational Therapies, IMRT & TG142 Highlights and selected product information only. A complete TG142 brochure is available. For more information on
Photon beam dose distributions in 2D
 Photon beam dose distributions in 2D Sastry Vedam PhD DABR Introduction to Medical Physics III: Therapy Spring 2014 Acknowledgments! Narayan Sahoo PhD! Richard G Lane (Late) PhD 1 Overview! Evaluation
Photon beam dose distributions in 2D Sastry Vedam PhD DABR Introduction to Medical Physics III: Therapy Spring 2014 Acknowledgments! Narayan Sahoo PhD! Richard G Lane (Late) PhD 1 Overview! Evaluation
TPS COMMISSIONING. Laurence Court University of Texas MD Anderson Cancer Center 4/3/2017 1
 TPS COMMISSIONING Laurence Court University of Texas MD Anderson Cancer Center 4/3/2017 1 Conflicts of interest Court receives funding from NIH, CPIRT, Varian and Elekta 4/3/2017 2 Resources your first
TPS COMMISSIONING Laurence Court University of Texas MD Anderson Cancer Center 4/3/2017 1 Conflicts of interest Court receives funding from NIH, CPIRT, Varian and Elekta 4/3/2017 2 Resources your first
An Investigation of a Model of Percentage Depth Dose for Irregularly Shaped Fields
 Int. J. Cancer (Radiat. Oncol. Invest): 96, 140 145 (2001) 2001 Wiley-Liss, Inc. Publication of the International Union Against Cancer An Investigation of a Model of Percentage Depth Dose for Irregularly
Int. J. Cancer (Radiat. Oncol. Invest): 96, 140 145 (2001) 2001 Wiley-Liss, Inc. Publication of the International Union Against Cancer An Investigation of a Model of Percentage Depth Dose for Irregularly
Monte Carlo Simulation for Neptun 10 PC Medical Linear Accelerator and Calculations of Electron Beam Parameters
 Monte Carlo Simulation for Neptun 1 PC Medical Linear Accelerator and Calculations of Electron Beam Parameters M.T. Bahreyni Toossi a, M. Momen Nezhad b, S.M. Hashemi a a Medical Physics Research Center,
Monte Carlo Simulation for Neptun 1 PC Medical Linear Accelerator and Calculations of Electron Beam Parameters M.T. Bahreyni Toossi a, M. Momen Nezhad b, S.M. Hashemi a a Medical Physics Research Center,
Advanced Radiotherapy
 Advanced Radiotherapy IBA Concept for IMRT Verification Dr. Lutz Müller 1 IMRT Verification BIS BIS ADAS Fluence Model Delivered fluence Target Volume Constraints Inverse Backprojection Fluence Map Leaf
Advanced Radiotherapy IBA Concept for IMRT Verification Dr. Lutz Müller 1 IMRT Verification BIS BIS ADAS Fluence Model Delivered fluence Target Volume Constraints Inverse Backprojection Fluence Map Leaf
Clinical implementation of photon beam flatness measurements to verify beam quality
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Clinical implementation of photon beam flatness measurements to verify beam quality Simon Goodall, a Nicholas Harding, Jake Simpson,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Clinical implementation of photon beam flatness measurements to verify beam quality Simon Goodall, a Nicholas Harding, Jake Simpson,
3DVH : SUN NUCLEAR On The Accuracy Of The corporation Planned Dose Perturbation Algorithm Your Most Valuable QA and Dosimetry Tools *Patent Pending
 3DVH : On The Accuracy Of The Planned Dose Perturbation Algorithm SUN NUCLEAR corporation Your Most Valuable QA and Dosimetry Tools *Patent Pending introduction State-of-the-art IMRT QA of static gantry
3DVH : On The Accuracy Of The Planned Dose Perturbation Algorithm SUN NUCLEAR corporation Your Most Valuable QA and Dosimetry Tools *Patent Pending introduction State-of-the-art IMRT QA of static gantry
Effects of the difference in tube voltage of the CT scanner on. dose calculation
 Effects of the difference in tube voltage of the CT scanner on dose calculation Dong Joo Rhee, Sung-woo Kim, Dong Hyeok Jeong Medical and Radiological Physics Laboratory, Dongnam Institute of Radiological
Effects of the difference in tube voltage of the CT scanner on dose calculation Dong Joo Rhee, Sung-woo Kim, Dong Hyeok Jeong Medical and Radiological Physics Laboratory, Dongnam Institute of Radiological
4 Measurement. and Analysis. 4.1 Overview and Underlying Principles 4-1
 Measurement and Analysis.1 Overview and Underlying Principles.1.1 Introductory Remarks The physics and setup for film dosimetry have been described in the previous chapters. The measurement setup for IMRT
Measurement and Analysis.1 Overview and Underlying Principles.1.1 Introductory Remarks The physics and setup for film dosimetry have been described in the previous chapters. The measurement setup for IMRT
The MSKCC Approach to IMRT. Outline
 The MSKCC Approach to IMRT Spiridon V. Spirou, PhD Department of Medical Physics Memorial Sloan-Kettering Cancer Center New York, NY Outline Optimization Field splitting Delivery Independent verification
The MSKCC Approach to IMRT Spiridon V. Spirou, PhD Department of Medical Physics Memorial Sloan-Kettering Cancer Center New York, NY Outline Optimization Field splitting Delivery Independent verification
MapCHECK 2 & 3DVH. The Gold Standard for 2D Arrays
 MapCHECK 2 & 3DVH The Gold Standard for 2D Arrays Your Most Valuable QA and Dosimetry Tools THE GOLD STANDARD FOR 2D ARRAYS The MapCHECK 2 is the world s most selected independent 2D measurement array.
MapCHECK 2 & 3DVH The Gold Standard for 2D Arrays Your Most Valuable QA and Dosimetry Tools THE GOLD STANDARD FOR 2D ARRAYS The MapCHECK 2 is the world s most selected independent 2D measurement array.
MapCHECK 2 & 3DVH The Gold Standard for 2D Arrays
 MapCHECK 2 & 3DVH The Gold Standard for 2D Arrays Your Most Valuable QA and Dosimetry Tools THE GOLD STANDARD FOR 2D ARRAYS The MapCHECK 2 is the world s most selected independent 2D measurement array.
MapCHECK 2 & 3DVH The Gold Standard for 2D Arrays Your Most Valuable QA and Dosimetry Tools THE GOLD STANDARD FOR 2D ARRAYS The MapCHECK 2 is the world s most selected independent 2D measurement array.
Follow this and additional works at:
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2010 Implementation of the Dosimetry Check software package in computing 3D patient exit dose through generation
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2010 Implementation of the Dosimetry Check software package in computing 3D patient exit dose through generation
Dose Distributions. Purpose. Isodose distributions. To familiarize the resident with dose distributions and the factors that affect them
 Dose Distributions George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Purpose To familiarize the resident with dose distributions and the factors that affect them
Dose Distributions George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Purpose To familiarize the resident with dose distributions and the factors that affect them
MCNP4C3-BASED SIMULATION OF A MEDICAL LINEAR ACCELERATOR
 Computational Medical Physics Working Group Workshop II, Sep 3 Oct 3, 7 University of Florida (UF), Gainesville, Florida USA on CD-ROM, American Nuclear Society, LaGrange Park, IL (7) MCNP4C3-BASED SIMULATION
Computational Medical Physics Working Group Workshop II, Sep 3 Oct 3, 7 University of Florida (UF), Gainesville, Florida USA on CD-ROM, American Nuclear Society, LaGrange Park, IL (7) MCNP4C3-BASED SIMULATION
Evaluation of the magnitude of EBT Gafchromic film polarization effects
 Australasian Physical & Engineering Sciences in Medicine Volume 32 Number, 29 SCIENTIFIC NOTE Evaluation of the magnitude of EBT Gafchromic film polarization effects M. J. Butson,2, T. Cheung and P. K.
Australasian Physical & Engineering Sciences in Medicine Volume 32 Number, 29 SCIENTIFIC NOTE Evaluation of the magnitude of EBT Gafchromic film polarization effects M. J. Butson,2, T. Cheung and P. K.
Dynalog data tool for IMRT plan verification
 Dynalog data tool for IMRT plan verification Poster No.: R-0051 Congress: 2014 CSM Type: Scientific Exhibit Authors: V. Sashin; FOOTSCRAY/AU Keywords: Computer applications, Radiation physics, Experimental,
Dynalog data tool for IMRT plan verification Poster No.: R-0051 Congress: 2014 CSM Type: Scientific Exhibit Authors: V. Sashin; FOOTSCRAY/AU Keywords: Computer applications, Radiation physics, Experimental,
IMRT and VMAT Patient Specific QA Using 2D and 3D Detector Arrays
 IMRT and VMAT Patient Specific QA Using 2D and 3D Detector Arrays Sotiri Stathakis Outline Why IMRT/VMAT QA AAPM TG218 UPDATE Tolerance Limits and Methodologies for IMRT Verification QA Common sources
IMRT and VMAT Patient Specific QA Using 2D and 3D Detector Arrays Sotiri Stathakis Outline Why IMRT/VMAT QA AAPM TG218 UPDATE Tolerance Limits and Methodologies for IMRT Verification QA Common sources
Use of Monte Carlo modelling in radiotherapy linac design. David Roberts, PhD Senior Physicist Elekta
 Use of Monte Carlo modelling in radiotherapy linac design David Roberts, PhD Senior Physicist Elekta Contents Overview of Elekta What we do Where we use Monte Carlo Codes and resources Example : Agility
Use of Monte Carlo modelling in radiotherapy linac design David Roberts, PhD Senior Physicist Elekta Contents Overview of Elekta What we do Where we use Monte Carlo Codes and resources Example : Agility
Acknowledgments. Ping Xia, Ph.D., UCSF. Pam Akazawa, CMD, UCSF. Cynthia Chuang, Ph.D., UCSF
 Page 1 Quality Assurance of IMRT Delivery Systems - Siemens Lynn J. Verhey, Ph.D. Professor and Vice-Chair UCSF Dept. of Radiation Oncology AAPM 22 Annual Meeting, Montreal Acknowledgments Ping Xia, Ph.D.,
Page 1 Quality Assurance of IMRT Delivery Systems - Siemens Lynn J. Verhey, Ph.D. Professor and Vice-Chair UCSF Dept. of Radiation Oncology AAPM 22 Annual Meeting, Montreal Acknowledgments Ping Xia, Ph.D.,
VALIDATION OF A MONTE CARLO DOSE CALCULATION ALGORITHM FOR CLINICAL ELECTRON BEAMS IN THE PRESENCE OF PHANTOMS WITH COMPLEX HETEROGENEITIES
 VALIDATION OF A MONTE CARLO DOSE CALCULATION ALGORITHM FOR CLINICAL ELECTRON BEAMS IN THE PRESENCE OF PHANTOMS WITH COMPLEX HETEROGENEITIES by Shayla Landfair Enright A Thesis Submitted to the Faculty
VALIDATION OF A MONTE CARLO DOSE CALCULATION ALGORITHM FOR CLINICAL ELECTRON BEAMS IN THE PRESENCE OF PHANTOMS WITH COMPLEX HETEROGENEITIES by Shayla Landfair Enright A Thesis Submitted to the Faculty
CBCT Equivalent Source Generation Using HVL and Beam Profile Measurements. Johnny Little PSM - Medical Physics Graduate Student University of Arizona
 CBCT Equivalent Source Generation Using HVL and Beam Profile Measurements. Johnny Little PSM - Medical Physics Graduate Student University of Arizona Introduction CBCT has become a routine procedure for
CBCT Equivalent Source Generation Using HVL and Beam Profile Measurements. Johnny Little PSM - Medical Physics Graduate Student University of Arizona Introduction CBCT has become a routine procedure for
Raising the Bar in IMRT QA
 MapCHECK 2TM Raising the Bar in IMRT QA The leader in quick and precise measurement of modulated radiotherapy beams Benefits Proven solution for film-less rotational delivery and IMRT QA - More than 1500
MapCHECK 2TM Raising the Bar in IMRT QA The leader in quick and precise measurement of modulated radiotherapy beams Benefits Proven solution for film-less rotational delivery and IMRT QA - More than 1500
Implementation of the EGSnrc / BEAMnrc Monte Carlo code - Application to medical accelerator SATURNE43
 International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 6 No. 3 July 2014, pp. 635-641 2014 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ Implementation
International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 6 No. 3 July 2014, pp. 635-641 2014 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ Implementation
IMSURE QA SOFTWARE FAST, PRECISE QA SOFTWARE
 QA SOFTWARE FAST, PRECISE Software for accurate and independent verification of monitor units, dose, and overall validity of standard, IMRT, VMAT, SRS and brachytherapy plans no film, no phantoms, no linac
QA SOFTWARE FAST, PRECISE Software for accurate and independent verification of monitor units, dose, and overall validity of standard, IMRT, VMAT, SRS and brachytherapy plans no film, no phantoms, no linac
FAST, precise. qa software
 qa software FAST, precise Software for accurate and independent verification of monitor units, dose, and overall validity of standard, IMRT, rotational or brachytherapy plans no film, no phantoms, no linac
qa software FAST, precise Software for accurate and independent verification of monitor units, dose, and overall validity of standard, IMRT, rotational or brachytherapy plans no film, no phantoms, no linac
IMRT site-specific procedure: Prostate (CHHiP)
 IMRT site-specific procedure: Prostate (CHHiP) Scope: To provide site specific instructions for the planning of CHHIP IMRT patients Responsibilities: Radiotherapy Physicists, HPC Registered Therapy Radiographers
IMRT site-specific procedure: Prostate (CHHiP) Scope: To provide site specific instructions for the planning of CHHIP IMRT patients Responsibilities: Radiotherapy Physicists, HPC Registered Therapy Radiographers
Preface. Med. Phys. 35(9), , Mechanical QA. Radiation Survey Mechanical tests Light radiation Table, Collimator, Gantry Jaws.
 AAPM-SAM-2012-Das (1) Beam Data Collection and Commissioning for Linear Accelerators: Technical Considerations and Recommendations Preface Indra J. Das, PhD, FAAPM, FACR, FASTRO Department of Radiation
AAPM-SAM-2012-Das (1) Beam Data Collection and Commissioning for Linear Accelerators: Technical Considerations and Recommendations Preface Indra J. Das, PhD, FAAPM, FACR, FASTRO Department of Radiation
Transitioning from pencil beam to Monte Carlo for electron dose calculations
 Transitioning from pencil beam to Monte Carlo for electron dose calculations Jessie Huang-Vredevoogd (jyhuang4@wisc.edu) University of Wisconsin NCC AAPM October 12, 2019 1 Topics to cover Background RayStation
Transitioning from pencil beam to Monte Carlo for electron dose calculations Jessie Huang-Vredevoogd (jyhuang4@wisc.edu) University of Wisconsin NCC AAPM October 12, 2019 1 Topics to cover Background RayStation
Basics of treatment planning II
 Basics of treatment planning II Sastry Vedam PhD DABR Introduction to Medical Physics III: Therapy Spring 2015 Dose calculation algorithms! Correction based! Model based 1 Dose calculation algorithms!
Basics of treatment planning II Sastry Vedam PhD DABR Introduction to Medical Physics III: Therapy Spring 2015 Dose calculation algorithms! Correction based! Model based 1 Dose calculation algorithms!
Verification measurements of an emc algorithm using a 2D ion chamber array
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 17, NUMBER 5, 2016 Verification measurements of an emc algorithm using a 2D ion chamber array Mark D. Wanklyn, 1a Ghirmay Kidane, 2 and Liz Crees 2 Medical
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 17, NUMBER 5, 2016 Verification measurements of an emc algorithm using a 2D ion chamber array Mark D. Wanklyn, 1a Ghirmay Kidane, 2 and Liz Crees 2 Medical
UNCOMPROMISING QUALITY
 ION CHAMBERS UNCOMPROMISING QUALITY Designed with over 30 years of scientific integrity for a broad range of dosimetry measurements in diverse radiation beams Farmer-type Chambers For absolute dosimetry
ION CHAMBERS UNCOMPROMISING QUALITY Designed with over 30 years of scientific integrity for a broad range of dosimetry measurements in diverse radiation beams Farmer-type Chambers For absolute dosimetry
Proton dose calculation algorithms and configuration data
 Proton dose calculation algorithms and configuration data Barbara Schaffner PTCOG 46 Educational workshop in Wanjie, 20. May 2007 VARIAN Medical Systems Agenda Broad beam algorithms Concept of pencil beam
Proton dose calculation algorithms and configuration data Barbara Schaffner PTCOG 46 Educational workshop in Wanjie, 20. May 2007 VARIAN Medical Systems Agenda Broad beam algorithms Concept of pencil beam
A secondary monitor unit calculation algorithm using superposition of symmetric, open fields for IMRT plans
 Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2013 A secondary monitor unit calculation algorithm using superposition of symmetric, open fields for IMRT plans Adam
Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2013 A secondary monitor unit calculation algorithm using superposition of symmetric, open fields for IMRT plans Adam
Graphical Analysis of Data using Microsoft Excel [2016 Version]
![Graphical Analysis of Data using Microsoft Excel [2016 Version] Graphical Analysis of Data using Microsoft Excel [2016 Version]](/thumbs/72/67574169.jpg) Graphical Analysis of Data using Microsoft Excel [2016 Version] Introduction In several upcoming labs, a primary goal will be to determine the mathematical relationship between two variable physical parameters.
Graphical Analysis of Data using Microsoft Excel [2016 Version] Introduction In several upcoming labs, a primary goal will be to determine the mathematical relationship between two variable physical parameters.
Qalitätssicherung an Multileafkollimatoren. Dr. Lutz Müller Würzburg jan 2004
 Qalitätssicherung an Multileafkollimatoren Dr. Lutz Müller Würzburg jan 2004 IMRT Verification - present Target Volume Constraints Inverse Planning Algorithm Fluence Map Leaf Sequencer Leaf & Gantry sequence
Qalitätssicherung an Multileafkollimatoren Dr. Lutz Müller Würzburg jan 2004 IMRT Verification - present Target Volume Constraints Inverse Planning Algorithm Fluence Map Leaf Sequencer Leaf & Gantry sequence
THE SIMULATION OF THE 4 MV VARIAN LINAC WITH EXPERIMENTAL VALIDATION
 2007 International Nuclear Atlantic Conference - INAC 2007 Santos, SP, Brazil, September 30 to October 5, 2007 ASSOCIAÇÃO BRASILEIRA DE ENERGIA NUCLEAR - ABEN ISBN: 978-85-99141-02-1 THE SIMULATION OF
2007 International Nuclear Atlantic Conference - INAC 2007 Santos, SP, Brazil, September 30 to October 5, 2007 ASSOCIAÇÃO BRASILEIRA DE ENERGIA NUCLEAR - ABEN ISBN: 978-85-99141-02-1 THE SIMULATION OF
Using Excel for Graphical Analysis of Data
 Using Excel for Graphical Analysis of Data Introduction In several upcoming labs, a primary goal will be to determine the mathematical relationship between two variable physical parameters. Graphs are
Using Excel for Graphical Analysis of Data Introduction In several upcoming labs, a primary goal will be to determine the mathematical relationship between two variable physical parameters. Graphs are
Facility Questionnaire PART I (General Information for 3DCRT and IMRT)
 Facility Questionnaire PART I (General Information for 3DCRT and IMRT) The following items are required before you can enter cases on any RTOG protocol that requires data submission to the Image-Guided
Facility Questionnaire PART I (General Information for 3DCRT and IMRT) The following items are required before you can enter cases on any RTOG protocol that requires data submission to the Image-Guided
Intensity-modulated radiation therapy dose maps: the matchline effect
 University of Wollongong Research Online University of Wollongong Thesis Collection 1954-2016 University of Wollongong Thesis Collections 2006 Intensity-modulated radiation therapy dose maps: the matchline
University of Wollongong Research Online University of Wollongong Thesis Collection 1954-2016 University of Wollongong Thesis Collections 2006 Intensity-modulated radiation therapy dose maps: the matchline
IAEA-TECDOC-1583 Commissioning of Radiotherapy Treatment Planning Systems: Testing for Typical External Beam Treatment Techniques
 IAEA-TECDOC-1583 Commissioning of Radiotherapy Treatment Planning Systems: Testing for Typical External Beam Treatment Techniques Report of the Coordinated Research Project (CRP) on Development of Procedures
IAEA-TECDOC-1583 Commissioning of Radiotherapy Treatment Planning Systems: Testing for Typical External Beam Treatment Techniques Report of the Coordinated Research Project (CRP) on Development of Procedures
Volumetric Modulated Arc Therapy - Clinical Implementation. Outline. Acknowledgement. History of VMAT. IMAT Basics of IMAT
 Volumetric Modulated Arc Therapy - Clinical Implementation Daliang Cao, PhD, DABR Swedish Cancer Institute, Seattle, WA Acknowledgement David M. Shepard, Ph.D. Muhammad K. N. Afghan, Ph.D. Fan Chen, Ph.D.
Volumetric Modulated Arc Therapy - Clinical Implementation Daliang Cao, PhD, DABR Swedish Cancer Institute, Seattle, WA Acknowledgement David M. Shepard, Ph.D. Muhammad K. N. Afghan, Ph.D. Fan Chen, Ph.D.
EXTERNAL PHOTON BEAMS: PHYSICAL ASPECTS
 EXTERNAL PHOTON BEAMS: PHYSICAL ASPECTS E.B. PODGORSAK Department of Medical Physics, McGill University Health Centre, Montreal, Quebec, Canada 6.1. INTRODUCTION Radiotherapy procedures fall into two main
EXTERNAL PHOTON BEAMS: PHYSICAL ASPECTS E.B. PODGORSAK Department of Medical Physics, McGill University Health Centre, Montreal, Quebec, Canada 6.1. INTRODUCTION Radiotherapy procedures fall into two main
6-1 LECTURE #6: OPTICAL PROPERTIES OF SOLIDS. Basic question: How do solids interact with light? The answers are linked to:
 LECTURE #6: OPTICAL PROPERTIES OF SOLIDS Basic question: How do solids interact with light? The answers are linked to: Properties of light inside a solid Mechanisms behind light reflection, absorption
LECTURE #6: OPTICAL PROPERTIES OF SOLIDS Basic question: How do solids interact with light? The answers are linked to: Properties of light inside a solid Mechanisms behind light reflection, absorption
Mr. Chaobin Li China Lucky Film Corp. No. 6 Lekai South Street 6, Baoding, Hebei Province, PRC Tel.:
 Evaluation of the image quality of X-ray exposed radiographic film samples of Lucky Film L4 in standard AGFA NDT S machine processing (8 min cycle time) BAM reference Copy Customer BAM 8.3/7728a 1 st copy
Evaluation of the image quality of X-ray exposed radiographic film samples of Lucky Film L4 in standard AGFA NDT S machine processing (8 min cycle time) BAM reference Copy Customer BAM 8.3/7728a 1 st copy
ABSORBED DOSE MEASUREMENTS AND MCNP MODELING FOR THE LEKSELL GAMMA KNIFE. A Thesis. the Degree Master of Science in the. Yipeng Li, B.S.
 ABSORBED DOSE MEASUREMENTS AND MCNP MODELING FOR THE LEKSELL GAMMA KNIFE A Thesis Presented in Partial Fulfillment of the Requirement for the Degree Master of Science in the Graduate School of The Ohio
ABSORBED DOSE MEASUREMENTS AND MCNP MODELING FOR THE LEKSELL GAMMA KNIFE A Thesis Presented in Partial Fulfillment of the Requirement for the Degree Master of Science in the Graduate School of The Ohio
Analysis of Radiation Transport through Multileaf Collimators Using BEAMnrc Code
 American Journal of Biomedical Engineering 216, 6(4): 124-131 DOI: 1.5923/j.ajbe.21664.3 Analysis of Radiation Transport through Multileaf Collimators Using BEAMnrc Code Ankit Kajaria 1,*, Neeraj Sharma
American Journal of Biomedical Engineering 216, 6(4): 124-131 DOI: 1.5923/j.ajbe.21664.3 Analysis of Radiation Transport through Multileaf Collimators Using BEAMnrc Code Ankit Kajaria 1,*, Neeraj Sharma
Disclosure. Outline. Acknowledgments. Ping Xia, Ph.D., Page 1. LINAC and MLC QA for IMRT. Received research support from Siemens Medical Solutions
 LINAC and MLC QA for IMRT Ping Xia, Ph.D., Department of Radiation Oncology Disclosure Received research support from Siemens Medical Solutions University of California San Francisco Therapy Series (SAM)
LINAC and MLC QA for IMRT Ping Xia, Ph.D., Department of Radiation Oncology Disclosure Received research support from Siemens Medical Solutions University of California San Francisco Therapy Series (SAM)
PROVIDE A UNIFORM DOSE IN THE SMALL ANIMAL.
 Considerations in the Use of the RS 2000 X ray Irradiator for Biological Research (Primarily Small Animal, tissue, and cells) and the fallacy of the High KV spectrum. The performance goal for a small animal
Considerations in the Use of the RS 2000 X ray Irradiator for Biological Research (Primarily Small Animal, tissue, and cells) and the fallacy of the High KV spectrum. The performance goal for a small animal
CLINICAL ASPECTS OF COMPACT GANTRY DESIGNS
 CLINICAL ASPECTS OF COMPACT GANTRY DESIGNS J. Heese, J. Wulff, A. Winnebeck, A. Huggins, M. Schillo VARIAN PARTICLE THERAPY JUERGEN HEESE New gantry developments Viewpoint from user and vendor perspective
CLINICAL ASPECTS OF COMPACT GANTRY DESIGNS J. Heese, J. Wulff, A. Winnebeck, A. Huggins, M. Schillo VARIAN PARTICLE THERAPY JUERGEN HEESE New gantry developments Viewpoint from user and vendor perspective
Tomotherapy Physics. Machine Twinning and Quality Assurance. Emilie Soisson, MS
 Tomotherapy Physics Machine Twinning and Quality Assurance Emilie Soisson, MS Tomotherapy at UW- Madison Treating for nearly 5 years Up to ~45 patients a day on 2 tomo units Units twinned to facilitate
Tomotherapy Physics Machine Twinning and Quality Assurance Emilie Soisson, MS Tomotherapy at UW- Madison Treating for nearly 5 years Up to ~45 patients a day on 2 tomo units Units twinned to facilitate
Measurement of depth-dose of linear accelerator and simulation by use of Geant4 computer code
 reports of practical oncology and radiotherapy 1 5 (2 0 1 0) 64 68 available at www.sciencedirect.com journal homepage: http://www.rpor.eu/ Original article Measurement of depth-dose of linear accelerator
reports of practical oncology and radiotherapy 1 5 (2 0 1 0) 64 68 available at www.sciencedirect.com journal homepage: http://www.rpor.eu/ Original article Measurement of depth-dose of linear accelerator
Code of practice: Create a verification plan for OCTAVIUS Detector 729 in Philips Pinnacle³
 Technical Note D655.208.03/00 Code of practice: Create a verification plan for OCTAVIUS Detector 729 in There are basically three ways to carry out verification of IMRT fluences. For all options, it is
Technical Note D655.208.03/00 Code of practice: Create a verification plan for OCTAVIUS Detector 729 in There are basically three ways to carry out verification of IMRT fluences. For all options, it is
SUMMARY OF DENTAL MEASUREMENT PROCEDURES (Abridged Protocol)
 SUMMARY OF DENTAL MEASUREMENT PROCEDURES (Abridged Protocol) INTRAORAL IMAGING PROCEDURE Entrance Skin Exposure / Air Kerma To measure the typical intraoral Entrance Skin Exposure (ESE) and Entrance Skin
SUMMARY OF DENTAL MEASUREMENT PROCEDURES (Abridged Protocol) INTRAORAL IMAGING PROCEDURE Entrance Skin Exposure / Air Kerma To measure the typical intraoral Entrance Skin Exposure (ESE) and Entrance Skin
Tips and Guidance for Analyzing Data. Executive Summary
 Tips and Guidance for Analyzing Data Executive Summary This document has information and suggestions about three things: 1) how to quickly do a preliminary analysis of time-series data; 2) key things to
Tips and Guidance for Analyzing Data Executive Summary This document has information and suggestions about three things: 1) how to quickly do a preliminary analysis of time-series data; 2) key things to
Error Analysis, Statistics and Graphing
 Error Analysis, Statistics and Graphing This semester, most of labs we require us to calculate a numerical answer based on the data we obtain. A hard question to answer in most cases is how good is your
Error Analysis, Statistics and Graphing This semester, most of labs we require us to calculate a numerical answer based on the data we obtain. A hard question to answer in most cases is how good is your
Megan A. Wood, M.S. Under the direction of Larry DeWerd, Ph.D. University of Wisconsin Medical Radiation Research Center (UWMRRC)
 Megan A. Wood, M.S. Under the direction of Larry DeWerd, Ph.D. University of Wisconsin Medical Radiation Research Center (UWMRRC) NCCAAPM Spring Meeting May 3, 2013 Introduction FFF background Project
Megan A. Wood, M.S. Under the direction of Larry DeWerd, Ph.D. University of Wisconsin Medical Radiation Research Center (UWMRRC) NCCAAPM Spring Meeting May 3, 2013 Introduction FFF background Project
225L Acceleration of Gravity and Measurement Statistics
 225L Acceleration of Gravity and Measurement Statistics Introduction: The most important and readily available source of acceleration has been gravity, and in particular, free fall. One of the problems
225L Acceleration of Gravity and Measurement Statistics Introduction: The most important and readily available source of acceleration has been gravity, and in particular, free fall. One of the problems
Helical Tomotherapy Qualitative dose Delivery Verification
 University of Tennessee, Knoxville Trace: Tennessee Research and Creative Exchange University of Tennessee Honors Thesis Projects University of Tennessee Honors Program 5-2003 Helical Tomotherapy Qualitative
University of Tennessee, Knoxville Trace: Tennessee Research and Creative Exchange University of Tennessee Honors Thesis Projects University of Tennessee Honors Program 5-2003 Helical Tomotherapy Qualitative
Spiral CT. Protocol Optimization & Quality Assurance. Ge Wang, Ph.D. Department of Radiology University of Iowa Iowa City, Iowa 52242, USA
 Spiral CT Protocol Optimization & Quality Assurance Ge Wang, Ph.D. Department of Radiology University of Iowa Iowa City, Iowa 52242, USA Spiral CT Protocol Optimization & Quality Assurance Protocol optimization
Spiral CT Protocol Optimization & Quality Assurance Ge Wang, Ph.D. Department of Radiology University of Iowa Iowa City, Iowa 52242, USA Spiral CT Protocol Optimization & Quality Assurance Protocol optimization
THE WIRELESS PHANTOM PERFORM ACCURATE PATIENT QA IN LESS TIME THAN EVER!
 THE WIRELESS PHANTOM PERFORM ACCURATE PATIENT QA IN LESS TIME THAN EVER! Confidence in complex treatments Modern radiation therapy uses complex plans with techniques such as IMRT, VMAT and Tomotherapy.
THE WIRELESS PHANTOM PERFORM ACCURATE PATIENT QA IN LESS TIME THAN EVER! Confidence in complex treatments Modern radiation therapy uses complex plans with techniques such as IMRT, VMAT and Tomotherapy.
Thank-You Members of TG147 TG 147: QA for nonradiographic
 Thank-You Members of TG147 TG 147: QA for nonradiographic localization and positioning systems Twyla Willoughby, M.S. Medical Physicist Clinical AAPM Meeting March 2013 Department of Radiation Oncology
Thank-You Members of TG147 TG 147: QA for nonradiographic localization and positioning systems Twyla Willoughby, M.S. Medical Physicist Clinical AAPM Meeting March 2013 Department of Radiation Oncology
DAILY LINAC QA BEAM QA
 BEAM QA DAILY LINAC QA The QA BeamChecker Plus allows for fast, reliable, and uncomplicated daily QA of Varian, Elekta, Siemens, and Accuray Treatment Machines. The QA BeamChecker Plus is specifically
BEAM QA DAILY LINAC QA The QA BeamChecker Plus allows for fast, reliable, and uncomplicated daily QA of Varian, Elekta, Siemens, and Accuray Treatment Machines. The QA BeamChecker Plus is specifically
Image Acquisition Systems
 Image Acquisition Systems Goals and Terminology Conventional Radiography Axial Tomography Computer Axial Tomography (CAT) Magnetic Resonance Imaging (MRI) PET, SPECT Ultrasound Microscopy Imaging ITCS
Image Acquisition Systems Goals and Terminology Conventional Radiography Axial Tomography Computer Axial Tomography (CAT) Magnetic Resonance Imaging (MRI) PET, SPECT Ultrasound Microscopy Imaging ITCS
WINdose for Excel 2002
 WINdose for Excel 2002 Installation & Operations Manual REQUIREMENTS WINdose for Excel 2002 is designed in a Microsoft Excel platform. WINdose for Excel 2002 was developed and intended for use as a component
WINdose for Excel 2002 Installation & Operations Manual REQUIREMENTS WINdose for Excel 2002 is designed in a Microsoft Excel platform. WINdose for Excel 2002 was developed and intended for use as a component
Chapter 7 Feasibility Study for 3D Online Motion Compensation
 Chapter 7 Feasibility Study for 3D Online Motion Compensation The current section presents the results of the experimental study of the feasibility of three-dimensional motion online compensation (3D-OMC)
Chapter 7 Feasibility Study for 3D Online Motion Compensation The current section presents the results of the experimental study of the feasibility of three-dimensional motion online compensation (3D-OMC)
How would, or how does, the patient position (chin extended) affect your beam arrangement?
 1 Megan Sullivan Clinical Practicum II Parotid Lab July 29, 2016 PLAN 1: IPSILATERAL WEDGE PAIR TECHNIQUE The ipsilateral wedge pair technique consisted of an anterior oblique field at 45 degrees and a
1 Megan Sullivan Clinical Practicum II Parotid Lab July 29, 2016 PLAN 1: IPSILATERAL WEDGE PAIR TECHNIQUE The ipsilateral wedge pair technique consisted of an anterior oblique field at 45 degrees and a
Impact of Multileaf Collimator Configuration Parameters on the Dosimetric Accuracy of 6-Mv Intensity-Modulated Radiation Therapy Treatment Plans
 Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2015 Impact of Multileaf Collimator Configuration Parameters on the Dosimetric Accuracy of 6-Mv Intensity-Modulated Radiation
Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2015 Impact of Multileaf Collimator Configuration Parameters on the Dosimetric Accuracy of 6-Mv Intensity-Modulated Radiation
A comparative analysis for verification of IMRT and VMAT treatment plans using a 2-D and 3-D diode array
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2014 A comparative analysis for verification of IMRT and VMAT treatment plans using a 2-D and 3-D diode array
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2014 A comparative analysis for verification of IMRT and VMAT treatment plans using a 2-D and 3-D diode array
7/31/2011. Learning Objective. Video Positioning. 3D Surface Imaging by VisionRT
 CLINICAL COMMISSIONING AND ACCEPTANCE TESTING OF A 3D SURFACE MATCHING SYSTEM Hania Al-Hallaq, Ph.D. Assistant Professor Radiation Oncology The University of Chicago Learning Objective Describe acceptance
CLINICAL COMMISSIONING AND ACCEPTANCE TESTING OF A 3D SURFACE MATCHING SYSTEM Hania Al-Hallaq, Ph.D. Assistant Professor Radiation Oncology The University of Chicago Learning Objective Describe acceptance
NEW METHOD OF COLLECTING OUTPUT FACTORS FOR COMMISSIONING LINEAR ACCELERATORS WITH SPECIAL EMPHASIS
 NEW METHOD OF COLLECTING OUTPUT FACTORS FOR COMMISSIONING LINEAR ACCELERATORS WITH SPECIAL EMPHASIS ON SMALL FIELDS AND INTENSITY MODULATED RADIATION THERAPY by Cindy D. Smith A Thesis Submitted to the
NEW METHOD OF COLLECTING OUTPUT FACTORS FOR COMMISSIONING LINEAR ACCELERATORS WITH SPECIAL EMPHASIS ON SMALL FIELDS AND INTENSITY MODULATED RADIATION THERAPY by Cindy D. Smith A Thesis Submitted to the
CHAPTER 2 MEDICAL IMAGING WITH NON-IONIZING RADIATION
 CHAPTER 2 MEDICAL IMAGING WITH NON-IONIZING RADIATION 1 Ultrasound Imaging 1.1 Ultrasound Production and Detection Ultrasound is frequency vibration. To produce and detect ultrasound, we use crystals which
CHAPTER 2 MEDICAL IMAGING WITH NON-IONIZING RADIATION 1 Ultrasound Imaging 1.1 Ultrasound Production and Detection Ultrasound is frequency vibration. To produce and detect ultrasound, we use crystals which
The use of an on-board MV imager for plan verification of intensity modulated radiation therapy and volumetrically modulated arc therapy
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2013 The use of an on-board MV imager for plan verification of intensity modulated radiation therapy and volumetrically
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2013 The use of an on-board MV imager for plan verification of intensity modulated radiation therapy and volumetrically
RITtrend allows you to effectively manage all your physics QA data in one powerful and customizable package.
 So much is asked of medical physicists these days We Can Help Automated Radiation Therapy Phantom Analysis in Seconds QC for Therapy OBI s and CT simulators. Radia s Catphan/OBI module performs analysis
So much is asked of medical physicists these days We Can Help Automated Radiation Therapy Phantom Analysis in Seconds QC for Therapy OBI s and CT simulators. Radia s Catphan/OBI module performs analysis
1. Learn to incorporate QA for surface imaging
 Hania Al-Hallaq, Ph.D. Assistant Professor Radiation Oncology The University of Chicago ***No disclosures*** 1. Learn to incorporate QA for surface imaging into current QA procedures for IGRT. 2. Understand
Hania Al-Hallaq, Ph.D. Assistant Professor Radiation Oncology The University of Chicago ***No disclosures*** 1. Learn to incorporate QA for surface imaging into current QA procedures for IGRT. 2. Understand
Air Kerma Strength Measurements and Monte Carlo based Dosimetric Characterization of a directional Pd 103 planar source array.
 Air Kerma Strength Measurements and Monte Carlo based Dosimetric Characterization of a directional Pd 103 planar source array. MANIK AIMA UWMRRC, MADISON 2014 NCAAPM Autumn Meeting October 24 th, 2014
Air Kerma Strength Measurements and Monte Carlo based Dosimetric Characterization of a directional Pd 103 planar source array. MANIK AIMA UWMRRC, MADISON 2014 NCAAPM Autumn Meeting October 24 th, 2014
Dealing with Data in Excel 2013/2016
 Dealing with Data in Excel 2013/2016 Excel provides the ability to do computations and graphing of data. Here we provide the basics and some advanced capabilities available in Excel that are useful for
Dealing with Data in Excel 2013/2016 Excel provides the ability to do computations and graphing of data. Here we provide the basics and some advanced capabilities available in Excel that are useful for
Design and performance characteristics of a Cone Beam CT system for Leksell Gamma Knife Icon
 Design and performance characteristics of a Cone Beam CT system for Leksell Gamma Knife Icon WHITE PAPER Introduction Introducing an image guidance system based on Cone Beam CT (CBCT) and a mask immobilization
Design and performance characteristics of a Cone Beam CT system for Leksell Gamma Knife Icon WHITE PAPER Introduction Introducing an image guidance system based on Cone Beam CT (CBCT) and a mask immobilization
Development a simple point source model for Elekta SL-25 linear accelerator using MCNP4C Monte Carlo code
 Iran. J. Radiat. Res., 2006; 4 (1): 7-14 Development a simple point source model for Elekta SL-25 linear accelerator using MCNP4C Monte Carlo code. Mesbahi * Department of Medical Physics, Medical School,
Iran. J. Radiat. Res., 2006; 4 (1): 7-14 Development a simple point source model for Elekta SL-25 linear accelerator using MCNP4C Monte Carlo code. Mesbahi * Department of Medical Physics, Medical School,
The IORT Treatment Planning System. radiance. GMV, 2012 Property of GMV All rights reserved
 The IORT Treatment Planning System radiance Property of GMV All rights reserved WHY RADIANCE? JUSTIFICATION Property of GMV All rights reserved ADVANTAGES OF IORT PRECISION: RT guided by direct vision.
The IORT Treatment Planning System radiance Property of GMV All rights reserved WHY RADIANCE? JUSTIFICATION Property of GMV All rights reserved ADVANTAGES OF IORT PRECISION: RT guided by direct vision.
A Method for Producing Simulated Mammograms: Observer Study
 A Method for Producing Simulated Mammograms: Observer Study Payam Seifi M.Sc. Michael R. Chinander Ph.D. Robert M. Nishikawa Ph.D., FAAPM Carl J. Vyborny Translational Laboratory for Breast Imaging Research
A Method for Producing Simulated Mammograms: Observer Study Payam Seifi M.Sc. Michael R. Chinander Ph.D. Robert M. Nishikawa Ph.D., FAAPM Carl J. Vyborny Translational Laboratory for Breast Imaging Research
CODE Analysis, design, production control of thin films
 M.Theiss Hard- and Software for Optical Spectroscopy Dr.-Bernhard-Klein-Str. 110, D-52078 Aachen Phone: (49) 241 5661390 Fax: (49) 241 9529100 E-mail: theiss@mtheiss.com Web: www.mtheiss.com CODE Analysis,
M.Theiss Hard- and Software for Optical Spectroscopy Dr.-Bernhard-Klein-Str. 110, D-52078 Aachen Phone: (49) 241 5661390 Fax: (49) 241 9529100 E-mail: theiss@mtheiss.com Web: www.mtheiss.com CODE Analysis,
The Finder Book for the Standard Celeration Chart
 Page The Finder Book for the Standard Celeration Chart Owen R. White University of Washington 22 Page 2 Introduction This book is designed to provide an overview of the Finder a device for finding frequencies,
Page The Finder Book for the Standard Celeration Chart Owen R. White University of Washington 22 Page 2 Introduction This book is designed to provide an overview of the Finder a device for finding frequencies,
A Geant4 based treatment plan verification tool: commissioning of the LINAC model and DICOM-RT interface
 A Geant4 based treatment plan verification tool: commissioning of the LINAC model and DICOM-RT interface Iwan Cornelius, Chris Poole. Stephen Warwick, Christian Langton Discipline of Physics, Faculty of
A Geant4 based treatment plan verification tool: commissioning of the LINAC model and DICOM-RT interface Iwan Cornelius, Chris Poole. Stephen Warwick, Christian Langton Discipline of Physics, Faculty of
ADVANCING CANCER TREATMENT
 The RayPlan treatment planning system makes proven, innovative RayStation technology accessible to clinics that need a cost-effective and streamlined solution. Fast, efficient and straightforward to use,
The RayPlan treatment planning system makes proven, innovative RayStation technology accessible to clinics that need a cost-effective and streamlined solution. Fast, efficient and straightforward to use,
Reading: Graphing Techniques Revised 1/12/11 GRAPHING TECHNIQUES
 GRAPHING TECHNIQUES Mathematical relationships between variables are determined by graphing experimental data. For example, the linear relationship between the concentration and the absorption of dilute
GRAPHING TECHNIQUES Mathematical relationships between variables are determined by graphing experimental data. For example, the linear relationship between the concentration and the absorption of dilute
Outline. Outline 7/24/2014. Fast, near real-time, Monte Carlo dose calculations using GPU. Xun Jia Ph.D. GPU Monte Carlo. Clinical Applications
 Fast, near real-time, Monte Carlo dose calculations using GPU Xun Jia Ph.D. xun.jia@utsouthwestern.edu Outline GPU Monte Carlo Clinical Applications Conclusions 2 Outline GPU Monte Carlo Clinical Applications
Fast, near real-time, Monte Carlo dose calculations using GPU Xun Jia Ph.D. xun.jia@utsouthwestern.edu Outline GPU Monte Carlo Clinical Applications Conclusions 2 Outline GPU Monte Carlo Clinical Applications
Comparison of absorbed dose distribution 10 MV photon beam on water phantom using Monte Carlo method and Analytical Anisotropic Algorithm
 Journal of Physics: Conference Series PAPER OPEN ACCESS Comparison of absorbed dose distribution 1 MV photon beam on water phantom using Monte Carlo method and Analytical Anisotropic Algorithm To cite
Journal of Physics: Conference Series PAPER OPEN ACCESS Comparison of absorbed dose distribution 1 MV photon beam on water phantom using Monte Carlo method and Analytical Anisotropic Algorithm To cite
A Customized Bolus Produced Using a 3-Dimensional Printer for Radiotherapy
 A Customized Bolus Produced Using a 3-Dimensional Printer for Radiotherapy Shin-Wook Kim, Hun-Joo Shin, Chul Seung Kay, Seok Hyun Son* Radiation Oncology, Incheon St. Mary s Hospital, College of Medicine,
A Customized Bolus Produced Using a 3-Dimensional Printer for Radiotherapy Shin-Wook Kim, Hun-Joo Shin, Chul Seung Kay, Seok Hyun Son* Radiation Oncology, Incheon St. Mary s Hospital, College of Medicine,
Outline. Monte Carlo Radiation Transport Modeling Overview (MCNP5/6) Monte Carlo technique: Example. Monte Carlo technique: Introduction
 Monte Carlo Radiation Transport Modeling Overview () Lecture 7 Special Topics: Device Modeling Outline Principles of Monte Carlo modeling Radiation transport modeling with Utilizing Visual Editor (VisEd)
Monte Carlo Radiation Transport Modeling Overview () Lecture 7 Special Topics: Device Modeling Outline Principles of Monte Carlo modeling Radiation transport modeling with Utilizing Visual Editor (VisEd)
Chapter 9 Field Shaping: Scanning Beam
 Chapter 9 Field Shaping: Scanning Beam X. Ronald Zhu, Ph.D. Department of Radiation Physics M. D. Anderson Cancer Center Houston, TX June 14-18, 2015 AAPM - Summer School 2015, Colorado Spring Acknowledgement
Chapter 9 Field Shaping: Scanning Beam X. Ronald Zhu, Ph.D. Department of Radiation Physics M. D. Anderson Cancer Center Houston, TX June 14-18, 2015 AAPM - Summer School 2015, Colorado Spring Acknowledgement
Three-dimensional dosimetry of small fields
 Three-dimensional of small fields Travis J. McCaw Medical Radiation Research Center Department of Medical Physics University of Wisconsin, Madison, WI NCCAAPM 2013 Fall Meeting 10 October 2013 Medical
Three-dimensional of small fields Travis J. McCaw Medical Radiation Research Center Department of Medical Physics University of Wisconsin, Madison, WI NCCAAPM 2013 Fall Meeting 10 October 2013 Medical
Spreadsheet Warm Up for SSAC Geology of National Parks Modules, 2: Elementary Spreadsheet Manipulations and Graphing Tasks
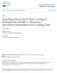 University of South Florida Scholar Commons Tampa Library Faculty and Staff Publications Tampa Library 2009 Spreadsheet Warm Up for SSAC Geology of National Parks Modules, 2: Elementary Spreadsheet Manipulations
University of South Florida Scholar Commons Tampa Library Faculty and Staff Publications Tampa Library 2009 Spreadsheet Warm Up for SSAC Geology of National Parks Modules, 2: Elementary Spreadsheet Manipulations
A study of densitometry comparison among three radiographic processing solutions
 Iran. J. Radiat. Res., 2006; 4 (2): 81-86 A study of densitometry comparison among three radiographic processing solutions V. Changizi 1*, E. Jazayeri 1,A.Talaeepour 2 1 Department of Radiology Technology,
Iran. J. Radiat. Res., 2006; 4 (2): 81-86 A study of densitometry comparison among three radiographic processing solutions V. Changizi 1*, E. Jazayeri 1,A.Talaeepour 2 1 Department of Radiology Technology,
