Eligibility and Benefits Inquiry & Claims Status Inquiry
|
|
|
- Osborne Knight
- 6 years ago
- Views:
Transcription
1 BlueExchange Guide Eligibility and Benefits Inquiry & Claims Status Inquiry Independence Blue Cross offers products directly, through Page its 1 subsidiaries of 8 Keystone Health Plan East and QCC Insurance Company, and with Highmark Blue Shield independent licensees of the Blue Cross and Blue Shield Association.
2 Eligibility and Benefits Inquiry The BlueExchange Eligibility and Benefits Inquiry transaction allows users to access up-to-date eligibility and benefits information for BlueCard out-of-area members. Note: If you are searching for benefits information for Independence Blue Cross (IBC) members, please use the Eligibility and Benefits Inquiry option from the Plan Transactions menu. To access the transaction, select BlueExchange (Out-of-Area) from the Plan Transactions menu, and then select Eligibility and Benefits Inquiry. The search screen appears: Steps to inquire about BlueExchange Eligibility and Benefits information for out-of-area members: 1. Enter your search criteria (see search criteria rules on page 4 for details). 2. Select Search. You will see one of the following: If one search result is returned: You will see the BlueExchange Eligibility and Benefits Details screen. If more than one search result is returned: You will see the BlueExchange Search Results screen. If eligibility details are unavailable: A message explaining why no details are available will appear. If applicable, retry your search using different search criteria (see search criteria rules on page 4 for details). Page 2 of 8
3 On the BlueExchange Eligibility and Benefits Search Results screen: If multiple members are displayed, click anywhere in the appropriate row in the results table to view the BlueExchange Eligibility and Benefits Details screen for that member. If you do not see the result you were searching for, select the Show Search Criteria link, edit your search criteria, and select Search (see search criteria rules on page 4 for details). On the BlueExchange Benefit Details screen, read the top portion of the screen for important information regarding this member's benefits, such as: member information subscriber information primary care provider other coverage service type Page 3 of 8
4 Search criteria rules NaviNet offers different search options for conducting a BlueExchange Eligibility and Benefits Inquiry. The following table shows the required fields based on search type: Search type Subscriber ID/ Date of Birth Subscriber ID/Name Required fields Subscriber ID Subscriber Date of Birth Selected Service Types Date of Service Subscriber ID Subscriber Last Name Subscriber First Name Selected Service Types Date of Service Tips: The three-character alpha prefix on the member ID card determines which Blues plan will receive the request. To search for Federal Employee Program (FEP) member information, enter the member ID number, including the preceding "R" in the Member ID field. For example, R If the alpha prefix identifies an IBC member, NaviNet will send an alert that directs you to use the Eligibility and Benefits Inquiry option from the Plan Transactions menu. The date of service defaults as today s date. The date of service can be up to two years in the past or up to six months in the future. This field must contain a date formatted as mm/dd/yyyy. You can still call the toll-free BlueCard Eligibility number BLUE (2583) with questions about out-of-area BlueCard members eligibility and benefits. Page 4 of 8
5 Claims Status Inquiry The BlueExchange Claim Status Inquiry transaction allows users to retrieve claims status information for BlueCard out-of-area members. To access the transaction, select BlueExchange (Out-of-Area) from the Plan Transactions menu, and then select Claim Status Inquiry. The search screen appears: Steps to inquire about claims status for out-of-area members: 1. Enter your search criteria (see search criteria rules on page 7 for details). 2. Select Search. You will see one of the following: If one search result is returned: You will see the BlueExchange Claim Status Details screen. If more than one search result is returned: You will see the BlueExchange Search Results screen. If claim details are unavailable: A message explaining why no details are available will appear. If applicable, retry your search using different search criteria (see search criteria rules on page 7 for details). Page 5 of 8
6 On the BlueExchange Claim Status Search Results screen: If you see the claim you are searching for, click the row in the results table to view the claim details screen. If you do not see the claim you were searching for, select the Show Search Criteria link, edit your search criteria, and select Search. On the BlueExchange Claim Status Details screen, view the screen for important information regarding this claim such as: patient information subscriber information provider information claim information definitions Page 6 of 8
7 Search Criteria Rules The required fields on the BlueExchange Claim Status Inquiry screen change depending on the "Patient Is" option that is selected: Patient Is Subscriber Dependent Required fields Billing Provider Subscriber ID Subscriber Last Name Subscriber Date of Birth Service Start Date Service End Date Billing Provider Subscriber ID Subscriber Last Name Dependent Last Name Dependent Date of Birth Service Start Date Service End Date Tips: On the BlueExchange Claim Status Inquiry Search screen: Subscriber IDs require the alpha prefix. If the alpha prefix identifies a local member, NaviNet will send an alert that directs you to use the Claim Status Inquiry option from the Plan Transactions menu. The Service Start Date defaults as three months prior to today's date. The Service End Date defaults to the current date. If inquiring on a facility claim, enter the Institutional Bill Type for a more successful search. If claim status details are not available, a message will appear indicating the reason. If the search criteria provide one result, you are taken directly to the BlueExchange Claim Status Details screen. If the search criteria provide more than one result, you are taken to the BlueExchange Search Results screen. On the BlueExchange Claim Status Inquiry Search Results screen: This screen displays up to 50 results. If more results are available, a message appears indicating that the maximum number of claims has been returned for the inquiry and that there may be additional claims that meet the criteria. Click on a patient in the search results table to select that claim and view the claim details. Page 7 of 8
8 If you do not see the claim you are searching for, use the Show Search Criteria link to narrow your search criteria and try again. NaviNet is a registered trademark of NaviNet, Inc., an independent company. The Blue Cross and Blue Shield names and symbols are registered marks of the Blue Cross and Blue Shield Association, an association of independent Blue Cross and Blue Shield plans. Page 8 of 8
BlueExchange Referral and Authorization Submission Guide
 BlueExchange Referral and Authorization Submission Guide Effective November 8, 2013 Independence Blue Cross offers products directly, through its subsidiaries Keystone Health Plan East and QCC Insurance
BlueExchange Referral and Authorization Submission Guide Effective November 8, 2013 Independence Blue Cross offers products directly, through its subsidiaries Keystone Health Plan East and QCC Insurance
Referral Submission and Inquiry Guide
 Referral Submission and Inquiry Guide Independence Blue Cross offers products directly, through Page its 1 subsidiaries of 10 Keystone Health Plan East and QCC Insurance Company, and with Highmark Blue
Referral Submission and Inquiry Guide Independence Blue Cross offers products directly, through Page its 1 subsidiaries of 10 Keystone Health Plan East and QCC Insurance Company, and with Highmark Blue
1500 Claim Submission Guide
 1500 Claim Submission Guide February 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East and QCC Insurance Company, and
1500 Claim Submission Guide February 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East and QCC Insurance Company, and
Referrals Guide. October Referrals Guide
 October 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East and QCC Insurance Company, and with Highmark Blue Shield independent
October 2016 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East and QCC Insurance Company, and with Highmark Blue Shield independent
Document Exchange Guide
 Document Exchange Guide April 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with
Document Exchange Guide April 2017 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and with
Authorization Submission and Inquiry Guide
 Authorization Submission and Inquiry Guide January 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Authorization Submission and Inquiry Guide January 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance
Note: For Single Sign-on (SSO) access for local contracted providers, please reference the tip sheet Pre-service Review for an out-of-area member.
 July 2016 The iexchange Web tool supports direct submission and provides online approval of benefits for preauthorization requests. Listed below are the steps for submitting a treatment search to Blue
July 2016 The iexchange Web tool supports direct submission and provides online approval of benefits for preauthorization requests. Listed below are the steps for submitting a treatment search to Blue
Referrals Guide. Referrals Guide. February AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Page Jersey 1 of 14
 Referrals Guide February 2018 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Page Jersey 1 of 14 The referral submission and inquiry transactions allow providers to submit new referrals for
Referrals Guide February 2018 AmeriHealth HMO, Inc. AmeriHealth Insurance Company of New Page Jersey 1 of 14 The referral submission and inquiry transactions allow providers to submit new referrals for
Provider File Management Guide
 Provider File Management Guide March 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and
Provider File Management Guide March 2018 Independence Blue Cross offers products through its subsidiaries Independence Hospital Indemnity Plan, Keystone Health Plan East, and QCC Insurance Company, and
Automated Information System AIS telephone user guide
 Automated Information System AIS telephone user guide May 2007 Department of Human Services Division of Medical Assistance Programs 500 Summer St NE, E 44 Salem, OR 97301-1077 1-800-527-5772 Contents I.
Automated Information System AIS telephone user guide May 2007 Department of Human Services Division of Medical Assistance Programs 500 Summer St NE, E 44 Salem, OR 97301-1077 1-800-527-5772 Contents I.
Massage therapy user guide
 Massage therapy user guide online claims submission... convenient service, delivered through an easy-to-use secure web site http://provider.ab.bluecross.ca/health September 2013 Massage therapy provider
Massage therapy user guide online claims submission... convenient service, delivered through an easy-to-use secure web site http://provider.ab.bluecross.ca/health September 2013 Massage therapy provider
Administrative Services of Kansas (ASK)
 Administrative Services of Kansas (ASK) HIPAA 276/277 005010X212 Standard Companion Guide Refers to the Implementation Guides Based on ASC X12 version 005010 January 2016 1 Disclosure Statement This document
Administrative Services of Kansas (ASK) HIPAA 276/277 005010X212 Standard Companion Guide Refers to the Implementation Guides Based on ASC X12 version 005010 January 2016 1 Disclosure Statement This document
Health Services provider user guide
 Health Services provider user guide online claims submission... convenient service, delivered through an easy-to-use secure web site http://provider.ab.bluecross.ca/health... convenient service, delivered
Health Services provider user guide online claims submission... convenient service, delivered through an easy-to-use secure web site http://provider.ab.bluecross.ca/health... convenient service, delivered
Interactive Voice Response System
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Interactive Voice Response System L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 0 2 P U B L I S H E D : J A N U A R Y 1 1,
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Interactive Voice Response System L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 0 2 P U B L I S H E D : J A N U A R Y 1 1,
Vx570 Transaction Guide New Jersey Medicaid Eligibility
 Healthcare Point-of-Service Transactions VeriFone Vx570 Terminals Vx570 Transaction Guide New Jersey Medicaid Eligibility Version March 1, 2013 Overview This transaction allows you to verify a patient
Healthcare Point-of-Service Transactions VeriFone Vx570 Terminals Vx570 Transaction Guide New Jersey Medicaid Eligibility Version March 1, 2013 Overview This transaction allows you to verify a patient
Super Care User Guide (Company)
 Super Care User Guide (Company) This material is for distribution in Hong Kong only. The distribution of this material is not and shall not be construed as an offer to sell or a solicitation to buy or
Super Care User Guide (Company) This material is for distribution in Hong Kong only. The distribution of this material is not and shall not be construed as an offer to sell or a solicitation to buy or
Welcome to the Blue Cross ilinkblue Training
 Welcome to the Blue Cross ilinkblue Training For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background noise (e.g.
Welcome to the Blue Cross ilinkblue Training For the listening benefit of webinar attendees, we have muted all lines and will be starting our presentation shortly This helps prevent background noise (e.g.
PROVIDER WEBSITE SITE ADMINISTRATOR GUIDE » PATIENT INQUIRY» CLAIM CENTER» FIND A DOCTOR» CLAIMS EDITING SYSTEM (CES)
 PROVIDER WEBSITE SITE ADMINISTRATOR GUIDE» PATIENT INQUIRY» CLAIM CENTER» FIND A DOCTOR» CLAIMS EDITING SYSTEM (CES) 2018 WPS Health Plan, Inc. 1 All rights reserved. JO7048 28898-085-1801 ADMINISTRATIVE
PROVIDER WEBSITE SITE ADMINISTRATOR GUIDE» PATIENT INQUIRY» CLAIM CENTER» FIND A DOCTOR» CLAIMS EDITING SYSTEM (CES) 2018 WPS Health Plan, Inc. 1 All rights reserved. JO7048 28898-085-1801 ADMINISTRATIVE
HPHConnect for Employers User s Guide
 HPHConnect for Employers User s Guide Copyright 2017 Harvard Pilgrim Health Care, Inc. All rights reserved. Harvard Pilgrim Health Care and the Harvard Pilgrim Health Care logo are trademarks of Harvard
HPHConnect for Employers User s Guide Copyright 2017 Harvard Pilgrim Health Care, Inc. All rights reserved. Harvard Pilgrim Health Care and the Harvard Pilgrim Health Care logo are trademarks of Harvard
Feature Articles. Effective March 14, 2011 The Premera clearinghouse will no longer accept other payers professional claims.
 EDI News July 2010 Contents Effective March 14, 2011 The Premera clearinghouse will no longer accept other payers professional claims. Feature Article page 1-2 Payer Updates page 3-4 Transactional Tips
EDI News July 2010 Contents Effective March 14, 2011 The Premera clearinghouse will no longer accept other payers professional claims. Feature Article page 1-2 Payer Updates page 3-4 Transactional Tips
Feature Articles. Effective March 14, 2011 The Premera clearinghouse will no longer accept other payers professional claims.
 EDI News July 2010 Contents Effective March 14, 2011 The Premera clearinghouse will no longer accept other payers professional claims. Feature Articles page 1 Payer Updates page 2-3 Transactional Tips
EDI News July 2010 Contents Effective March 14, 2011 The Premera clearinghouse will no longer accept other payers professional claims. Feature Articles page 1 Payer Updates page 2-3 Transactional Tips
270/271 Health Care Eligibility, Coverage, or Benefit Inquiry and Response
 Companion Document 270/271 270/271 Health Care Eligibility, Coverage, or Benefit Inquiry and Response Basic Instructions This section provides information to help you prepare for the ANSI ASC X12.281 Eligibility,
Companion Document 270/271 270/271 Health Care Eligibility, Coverage, or Benefit Inquiry and Response Basic Instructions This section provides information to help you prepare for the ANSI ASC X12.281 Eligibility,
HSA Contribution Guide. How to set up and send employer-directed HSA contributions
 HSA Guide How to set up and send employer-directed HSA contributions Table of contents Introduction...2 Employer contribution options...3 Getting started: Before you upload, run new reports to confirm
HSA Guide How to set up and send employer-directed HSA contributions Table of contents Introduction...2 Employer contribution options...3 Getting started: Before you upload, run new reports to confirm
Toll-free:
 Dear AeroVironment, Inc. Participants CoreSource Group # AE0000 Welcome! You have elected to participate in the AeroVironment, Inc Health Benefits Plan. CoreSource, Inc. is the Benefits Administrator for
Dear AeroVironment, Inc. Participants CoreSource Group # AE0000 Welcome! You have elected to participate in the AeroVironment, Inc Health Benefits Plan. CoreSource, Inc. is the Benefits Administrator for
epaces PA/DVS Response
 Version 2/Revision 2 Page 1 of 7 PA/DVS Activity Worklist You may view the list of PA/DVS Requests by clicking Responses under PA/DVS on the left-hand menu. This page has two sections the top contains
Version 2/Revision 2 Page 1 of 7 PA/DVS Activity Worklist You may view the list of PA/DVS Requests by clicking Responses under PA/DVS on the left-hand menu. This page has two sections the top contains
Provider Self-Service Tools
 Provider Self-Service Tools An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee of the Blue
Provider Self-Service Tools An independent licensee of the Blue Cross and Blue Shield Association. U7430a, 2/11 2012, Blue Cross and Blue Shield of North Carolina is an independent licensee of the Blue
< A symbol to indicate a value is less than another. For example, 2 < 3. This symbol is used in some BCBSNC proprietary error messages.
 Glossary < A symbol to indicate a value is less than another. For example, 2 < 3. This symbol is used in some BCBSNC proprietary error messages. > A symbol to indicate a value is greater than another.
Glossary < A symbol to indicate a value is less than another. For example, 2 < 3. This symbol is used in some BCBSNC proprietary error messages. > A symbol to indicate a value is greater than another.
AlwaysAssist User Guide Vision Care Provider Portal Page 0
 AlwaysAssist User Guide Vision Care Provider Portal Page 0 AlwaysAssist User Guide Vision Care Provider Portal Table of Contents Entering the Site... 2 Provider Login... 2 Password Change... 3 Password
AlwaysAssist User Guide Vision Care Provider Portal Page 0 AlwaysAssist User Guide Vision Care Provider Portal Table of Contents Entering the Site... 2 Provider Login... 2 Password Change... 3 Password
Electronic Explanation of Benefits Now Offered via My Account
 For Distribution to Brokers/General Producers/Full-Service Producers Only (Not Intended for Distribution to Groups and Members) November 1, 2011 Electronic Explanation of Benefits Now Offered via My Account
For Distribution to Brokers/General Producers/Full-Service Producers Only (Not Intended for Distribution to Groups and Members) November 1, 2011 Electronic Explanation of Benefits Now Offered via My Account
epaces - Claim Status Inquiry and Response
 Version 2/Revision 12 Page 1 of 7 Overview The Claim Status Inquiry function allows the User to inquire about the status of claims currently in the NYS Medicaid s adjudication process. The Claim Status
Version 2/Revision 12 Page 1 of 7 Overview The Claim Status Inquiry function allows the User to inquire about the status of claims currently in the NYS Medicaid s adjudication process. The Claim Status
Horizon BCBSNJ Broker Portal
 Horizon BCBSNJ Broker Portal User Guide VERSION 0.1 November 1, 2013 Contents 1 Introduction... 15 1.1 Overview... 15 1.2 Purpose... 15 1.3 Intended Audience... 15 1.4 Conventions Followed... 15 1.5 Structure
Horizon BCBSNJ Broker Portal User Guide VERSION 0.1 November 1, 2013 Contents 1 Introduction... 15 1.1 Overview... 15 1.2 Purpose... 15 1.3 Intended Audience... 15 1.4 Conventions Followed... 15 1.5 Structure
Netsmart Sandbox Tour Guide Script
 Netsmart Sandbox Tour Guide Script March 2012 This document is to be used in conjunction with the Netsmart Sandbox environment as a guide. Following the steps included in this guide will allow you to get
Netsmart Sandbox Tour Guide Script March 2012 This document is to be used in conjunction with the Netsmart Sandbox environment as a guide. Following the steps included in this guide will allow you to get
Administrative Manual
 Administrative Manual HealthLink Tools/Resources Chapter 10 1831 Chestnut Street St. Louis, MO 63103-2225 www.healthlink.com 1-877-284-0101 HealthLink Tools/Resources On-line Tools ProviderInfoSource HealthLink
Administrative Manual HealthLink Tools/Resources Chapter 10 1831 Chestnut Street St. Louis, MO 63103-2225 www.healthlink.com 1-877-284-0101 HealthLink Tools/Resources On-line Tools ProviderInfoSource HealthLink
Provider Website User Guide
 Provider Website User Guide Patient eligibility Claim search Find a Doctor Claims Editing System (CES) Secure messaging 2018 Wisconsin Physicians Service Insurance 1 Corporation. All rights reserved. JO9331
Provider Website User Guide Patient eligibility Claim search Find a Doctor Claims Editing System (CES) Secure messaging 2018 Wisconsin Physicians Service Insurance 1 Corporation. All rights reserved. JO9331
Colorado Access Provider Portal Guide
 Colorado Access Provider Portal Guide coaccess.com 1 CONTENTS INTRODUCTION... 3 SYSTEM REQUIREMENTS... 3 NEW PROVIDER REGISTRATION... 4 Provider Information... 4 New Provider Registration... 4 New Registration...
Colorado Access Provider Portal Guide coaccess.com 1 CONTENTS INTRODUCTION... 3 SYSTEM REQUIREMENTS... 3 NEW PROVIDER REGISTRATION... 4 Provider Information... 4 New Provider Registration... 4 New Registration...
Benefit Tracker. User Manual
 Benefit Tracker User Manual 2017 www.modahealth.com Revised 10/20/2017 Table of Contents Introduction Page 3 Benefit Tracker Overview Page 3 Security and Password Protection Page 3 Passwords Page 4 Getting
Benefit Tracker User Manual 2017 www.modahealth.com Revised 10/20/2017 Table of Contents Introduction Page 3 Benefit Tracker Overview Page 3 Security and Password Protection Page 3 Passwords Page 4 Getting
Version 1/Revision 7 Page 1 of 5. epaces - MEVS Eligibility Response
 Version 1/Revision 7 Page 1 of 5 Eligibility Response You may view the Eligibility Activity Worklist by clicking Responses under Eligibility on the left-hand menu. This page has two sections. The top section
Version 1/Revision 7 Page 1 of 5 Eligibility Response You may view the Eligibility Activity Worklist by clicking Responses under Eligibility on the left-hand menu. This page has two sections. The top section
Link 1500 / Online Claims Entry User Guide
 Link 1500 / Online Claims Entry User Guide ABILITY Network Inc Copyright and Trademark Copyright Copyright 2016 ABILITY Network Inc. All Rights Reserved. All text, images, and graphics, and other materials
Link 1500 / Online Claims Entry User Guide ABILITY Network Inc Copyright and Trademark Copyright Copyright 2016 ABILITY Network Inc. All Rights Reserved. All text, images, and graphics, and other materials
EmployerAccess online registration guide
 EmployerAccess online registration guide Register yourself and save time EmployerAccess enables you to manage your company-sponsored health plan efficiently using a simple, secure website. From one convenient
EmployerAccess online registration guide Register yourself and save time EmployerAccess enables you to manage your company-sponsored health plan efficiently using a simple, secure website. From one convenient
270/271 Eligibility Inquiry/Response
 270/271 Eligibility Inquiry/Response Overview... 1 Connectivity Transmission Options... 1 System Availability... 2 BlueCard and Federal Employee (FEP) Inquiries... 2 Eligibility Inquiry Processing... 2
270/271 Eligibility Inquiry/Response Overview... 1 Connectivity Transmission Options... 1 System Availability... 2 BlueCard and Federal Employee (FEP) Inquiries... 2 Eligibility Inquiry Processing... 2
278 Health Care Service Review and Response
 278 Health Care Service Review and Response Overview 2 Blue Card Inquiries (Blue Exchange) 2 Health Care Services Review Processing 2 Frequency of Data Exchange 2 Acknowledgements 2 Data Retention 3 Batch
278 Health Care Service Review and Response Overview 2 Blue Card Inquiries (Blue Exchange) 2 Health Care Services Review Processing 2 Frequency of Data Exchange 2 Acknowledgements 2 Data Retention 3 Batch
Employer Resource Center Training Guide
 Employer Resource Center Training Guide Version 3 July, 2013 Page 1 07/2013 Overview Purpose The purpose of this Training Guide is to provide you with some basic information how to use the Blue Cross and
Employer Resource Center Training Guide Version 3 July, 2013 Page 1 07/2013 Overview Purpose The purpose of this Training Guide is to provide you with some basic information how to use the Blue Cross and
2018 MEDICARE SUPPLEMENT RATES
 2018 MEDICARE SUPPLEMENT RATES ILLINOIS METRO Rates in the chart below correspond to the following ZIP codes. 60000-60110, 60114, 60116-60128, 60130-60134, 60136-60144, 60147-60149, 60152-60177, 60179-60399,
2018 MEDICARE SUPPLEMENT RATES ILLINOIS METRO Rates in the chart below correspond to the following ZIP codes. 60000-60110, 60114, 60116-60128, 60130-60134, 60136-60144, 60147-60149, 60152-60177, 60179-60399,
Provider Portal 3.0 Manual. Health Axis 3.0 Provider Portal User Guide
 Provider Portal 3.0 Manual Health Axis 3.0 Provider Portal User Guide Table of Contents Provider Portal 3.0... 4 How to Access the Provider Portal... 4 Login credentials:... 4 How to Request Access to
Provider Portal 3.0 Manual Health Axis 3.0 Provider Portal User Guide Table of Contents Provider Portal 3.0... 4 How to Access the Provider Portal... 4 Login credentials:... 4 How to Request Access to
Change Healthcare Provider Portal
 MED3000, a wholly owned subsidiary of Change Healthcare Change Healthcare Provider Portal Overview The provider portal provides secure, web-enabled, role-based access. You will be able to perform the following
MED3000, a wholly owned subsidiary of Change Healthcare Change Healthcare Provider Portal Overview The provider portal provides secure, web-enabled, role-based access. You will be able to perform the following
ABH Claims Entry System (ACES) Internet Claims System User Manual
 ABH Claims Entry System (ACES) Internet Claims System User Manual Advanced Behavioral Health, Inc. July 1, 2005 Table of Contents Login...3 Main Menu...4 File Submission...6 Claim Entry...8 HCFA1500...9
ABH Claims Entry System (ACES) Internet Claims System User Manual Advanced Behavioral Health, Inc. July 1, 2005 Table of Contents Login...3 Main Menu...4 File Submission...6 Claim Entry...8 HCFA1500...9
Pharmacist Resource Center User Guide
 Pharmacist Resource Center User Guide Purpose: This document is a step-by-step instruction guide for accessing the Pharmacist Resource Center functions. The Pharmacist Resource Center is an online tool
Pharmacist Resource Center User Guide Purpose: This document is a step-by-step instruction guide for accessing the Pharmacist Resource Center functions. The Pharmacist Resource Center is an online tool
Availity Remittance Viewer
 Availity Remittance Viewer August 2017 The Availity Remittance Viewer tool is an electronic solution that offers providers and billing services the ability to view, sort, save and print payment and remittance
Availity Remittance Viewer August 2017 The Availity Remittance Viewer tool is an electronic solution that offers providers and billing services the ability to view, sort, save and print payment and remittance
RETAIL PRODUCER PORTAL
 RETAIL PRODUCER PORTAL This presentation is a high-level summary and for general informational purposes only. The information in this presentation is not comprehensive and does not constitute legal, tax,
RETAIL PRODUCER PORTAL This presentation is a high-level summary and for general informational purposes only. The information in this presentation is not comprehensive and does not constitute legal, tax,
Reminder/Recall Notices
 From the Reports menu option, you may generate reminder and recall notices, which include letters, cards, address labels, client listings, and downloadable text files. Generation of reminder and recall
From the Reports menu option, you may generate reminder and recall notices, which include letters, cards, address labels, client listings, and downloadable text files. Generation of reminder and recall
What is mynas? How can you access mynas? Do I need to register to mynas? 1 How to use mynas
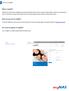 How to use mynas What is mynas? mynas is an online system designed to provide the Member with access to view their policy details, submit a re-imbursement claim, send inquirers, search for providers and
How to use mynas What is mynas? mynas is an online system designed to provide the Member with access to view their policy details, submit a re-imbursement claim, send inquirers, search for providers and
Provider Portal Training
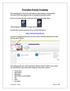 Provider Portal Training This training guide will provide information on the benefits of using NaviNet (Provider Portal) and a guide on how to navigate the NaviNet system. First, to access the provider
Provider Portal Training This training guide will provide information on the benefits of using NaviNet (Provider Portal) and a guide on how to navigate the NaviNet system. First, to access the provider
A handy reference for the S.C. Medicaid Web-based Claims Submission Tool: Lists (pg.1) History (pg. 3) Claims Entry (pg. 2)
 A handy reference for the S.C. Medicaid Web-based Claims Submission Tool: Lists (pg.1) History (pg. 3) Claims Entry (pg. 2) Eligibility (pg. 5) Claim Submission (pg.3) e-remits (pg.6) Status (pg. 4) Lists
A handy reference for the S.C. Medicaid Web-based Claims Submission Tool: Lists (pg.1) History (pg. 3) Claims Entry (pg. 2) Eligibility (pg. 5) Claim Submission (pg.3) e-remits (pg.6) Status (pg. 4) Lists
HealthKeepers, Inc. Website User Guide: Precertification Requests
 HealthKeepers, Inc. Website User Guide: Precertification Requests Services, Emergent Admissions and Maternity/OB Use our provider website to determine whether a service requires precertification and to
HealthKeepers, Inc. Website User Guide: Precertification Requests Services, Emergent Admissions and Maternity/OB Use our provider website to determine whether a service requires precertification and to
Accessing Blue Cross Secure Online Services (a training webinar for administrative representatives)
 Accessing Blue Cross Secure Online Services (a training webinar for administrative representatives) 2016-2017 Presented by Jami Zachary Provider Relations Department Blue Cross and Blue Shield of Louisiana
Accessing Blue Cross Secure Online Services (a training webinar for administrative representatives) 2016-2017 Presented by Jami Zachary Provider Relations Department Blue Cross and Blue Shield of Louisiana
Anthem Blue Cross and Blue Shield Serving Hoosier Healthwise, Healthy Indiana Plan and Hoosier Care Connect. Using the 2018 Availity Portal
 Serving Hoosier Healthwise, Healthy Indiana Plan Using the 2018 Availity Portal Agenda How to pull patient panel reports Interactive Care Reviewer (ICR) Submitting a request for prior authorization Viewing
Serving Hoosier Healthwise, Healthy Indiana Plan Using the 2018 Availity Portal Agenda How to pull patient panel reports Interactive Care Reviewer (ICR) Submitting a request for prior authorization Viewing
Helpful Hints: Request an Initial Authorization
 Helpful Hints: Request an Initial Authorization Select Location Select Location Window Patient Selection Referral Source Type Patient Last Name Patient First Name Patient DOB Insurance Name Subscriber
Helpful Hints: Request an Initial Authorization Select Location Select Location Window Patient Selection Referral Source Type Patient Last Name Patient First Name Patient DOB Insurance Name Subscriber
Use this task to submit an adoption life event in the UCPath website.
 Use this task to submit an adoption life event in the UCPath website. Marriage, birth, adoption, divorce and benefit changes for AD&D, disability insurance or life insurance can be made by the employee
Use this task to submit an adoption life event in the UCPath website. Marriage, birth, adoption, divorce and benefit changes for AD&D, disability insurance or life insurance can be made by the employee
ZIP CODE REQUIREMENT:
 HighMark Blue Cross Pennsylvania 5010 Information ANSI 4010 is the way you transmit electronic claims today. 5010 is the new ANSI electronic claim format Congress is requiring electronic claim billers
HighMark Blue Cross Pennsylvania 5010 Information ANSI 4010 is the way you transmit electronic claims today. 5010 is the new ANSI electronic claim format Congress is requiring electronic claim billers
Eaglesoft 16: Account
 Eaglesoft 16: Account Eaglesoft 16 offers a modernized Account window with sophisticated technology and improved functionality. Dockable panels and tabs make it easier than ever to navigate the Account
Eaglesoft 16: Account Eaglesoft 16 offers a modernized Account window with sophisticated technology and improved functionality. Dockable panels and tabs make it easier than ever to navigate the Account
837 Dental Health Care Claim
 Companion Document 837D 837 Dental Health Care Claim Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care transaction for dental claims. The remaining
Companion Document 837D 837 Dental Health Care Claim Basic Instructions This section provides information to help you prepare for the ANSI ASC X12N 837 Health Care transaction for dental claims. The remaining
Claims Portal. Updated: 1/25/13. Claims Portal Solely For HealthCare Partners i
 Updated: 1/25/13-2012 i Table of Contents Claims Online Portal Access... 3 Through PIP:... 3 Search Claims/Referrals... 5 By Patient Name... 5 Quick Search Claims/Referrals... 6 Advanced Search Claims/Referrals...
Updated: 1/25/13-2012 i Table of Contents Claims Online Portal Access... 3 Through PIP:... 3 Search Claims/Referrals... 5 By Patient Name... 5 Quick Search Claims/Referrals... 6 Advanced Search Claims/Referrals...
Connecticut Medical Assistance Program Web Guide Prior Authorization Search
 September 9, 014 Connecticut Medical Assistance Program Web Guide Prior Authorization Search The Prior Authorization (PA) Search process allows providers to submit a real-time transaction from the secure
September 9, 014 Connecticut Medical Assistance Program Web Guide Prior Authorization Search The Prior Authorization (PA) Search process allows providers to submit a real-time transaction from the secure
EmployerAccess. A step-by-step guide for managing your group benefits online. bcbsga.com GAEENBGA 12/17
 EmployerAccess A step-by-step guide for managing your group benefits online bcbsga.com 04377GAEENBGA /7 Table of contents Here s what EmployerAccess can do for you...................... 3 Getting started.......................................
EmployerAccess A step-by-step guide for managing your group benefits online bcbsga.com 04377GAEENBGA /7 Table of contents Here s what EmployerAccess can do for you...................... 3 Getting started.......................................
Physician Online Data System
 Physician Online Data System Medical Network One, PC 4986 Adams Rd., Suite D Rochester, MI 48306 Physician Online Data System (PODS) Register for PODS... 4 User name and password... 7 Login... 8 Member
Physician Online Data System Medical Network One, PC 4986 Adams Rd., Suite D Rochester, MI 48306 Physician Online Data System (PODS) Register for PODS... 4 User name and password... 7 Login... 8 Member
EmployerAccess online registration guide
 EmployerAccess online registration guide Register yourself and save time EmployerAccess enables you to manage your company-sponsored health plan efficiently using a simple, secure website. From one convenient
EmployerAccess online registration guide Register yourself and save time EmployerAccess enables you to manage your company-sponsored health plan efficiently using a simple, secure website. From one convenient
Frequently Asked Questions
 Q: Do any Qualifying Life Events (QLE) require documentation? If yes, how should they be submitted? A: There are five (5) QLEs that require documentation: 1. Over-age dependent 2. Adoption (within 31 days
Q: Do any Qualifying Life Events (QLE) require documentation? If yes, how should they be submitted? A: There are five (5) QLEs that require documentation: 1. Over-age dependent 2. Adoption (within 31 days
NaviNet Drug Authorizations. User s Guide
 NaviNet Drug Authorizations User s Guide NaviNet Drug Authorizations User s Guide 1 Overview NaviNet has partnered with CoverMyMeds to create NaviNet Drug Authorizations, an all-payer, HIPAA compliant
NaviNet Drug Authorizations User s Guide NaviNet Drug Authorizations User s Guide 1 Overview NaviNet has partnered with CoverMyMeds to create NaviNet Drug Authorizations, an all-payer, HIPAA compliant
Dental Connect Payers
 Dental Connect Payers User Guide 2.1 10/11/2017 Preface Preface Contents of the Change Healthcare documentation and software is copyrighted as a collective work under the laws of United States and other
Dental Connect Payers User Guide 2.1 10/11/2017 Preface Preface Contents of the Change Healthcare documentation and software is copyrighted as a collective work under the laws of United States and other
icare s Provider Portal Guide
 icare s Provider Portal Guide 2 CONTENTS New Provider Registration... 4 New Registration...5 Login Page 9 Sign In 9 Forget Your Password...10 Provider Home Page 12 Track Request 12 Contact Us.. 14 Provider
icare s Provider Portal Guide 2 CONTENTS New Provider Registration... 4 New Registration...5 Login Page 9 Sign In 9 Forget Your Password...10 Provider Home Page 12 Track Request 12 Contact Us.. 14 Provider
Trading Partner Account (TPA) User Guide. for. State of Idaho MMIS
 Trading Partner Account (TPA) User Guide for State of Idaho MMIS Date of Publication: 3/8/2018 Document Number: RF019 Version: 4.0 This document and information contains proprietary information and copyrighted
Trading Partner Account (TPA) User Guide for State of Idaho MMIS Date of Publication: 3/8/2018 Document Number: RF019 Version: 4.0 This document and information contains proprietary information and copyrighted
Claim Follow Up. Availity Customer Connection Availity, LLC All Rights Reserved
 Claim Follow Up Availity Customer Connection 2011 1 What We Will Cover Streamline administrative workflow with a single connection to multiple health plans for claim status, remittance, and review. 5010
Claim Follow Up Availity Customer Connection 2011 1 What We Will Cover Streamline administrative workflow with a single connection to multiple health plans for claim status, remittance, and review. 5010
Provider Maintenance Form
 Provider Maintenance Form March 2018 A quick and easy new way for Anthem providers to submit demographic updates online Submit demographic updates online The Provider Maintenance Form (PMF) is an online
Provider Maintenance Form March 2018 A quick and easy new way for Anthem providers to submit demographic updates online Submit demographic updates online The Provider Maintenance Form (PMF) is an online
A BETTER WAY TO TAKE CARE OF BUSINESS. Employers Online Enrollment Center Guide
 A BETTER WAY TO TAKE CARE OF BUSINESS Employers Online Enrollment Center Guide Quick Reference 3 What do you want to do? 3 Step-by-step guide 4 Sign on 4 Your landing page 5 Enroll new members 6 Add a
A BETTER WAY TO TAKE CARE OF BUSINESS Employers Online Enrollment Center Guide Quick Reference 3 What do you want to do? 3 Step-by-step guide 4 Sign on 4 Your landing page 5 Enroll new members 6 Add a
276/277 Claim Status Request and Response
 276/277 Claim Status Request and Response 276 & 277 Health Care Claim Status Request and Response 2 Overview 2 Connectivity Transmission Options 2 System Availability 3 Frequency of Data Exchange 3 Claim
276/277 Claim Status Request and Response 276 & 277 Health Care Claim Status Request and Response 2 Overview 2 Connectivity Transmission Options 2 System Availability 3 Frequency of Data Exchange 3 Claim
Emdeon Vision Payment Manager Integration. User Guide
 Emdeon Vision Payment Manager Integration User Guide Version 1 November, 2010 This page intentionally left blank. Vision - Payment Manager Integration Guide Copyright 1 Searching for ERAs 2 Sorting Columns...
Emdeon Vision Payment Manager Integration User Guide Version 1 November, 2010 This page intentionally left blank. Vision - Payment Manager Integration Guide Copyright 1 Searching for ERAs 2 Sorting Columns...
HSA Contribution Guide. How to set up and send employer-directed HSA contributions
 HSA Contribution Guide How to set up and send employer-directed HSA contributions Introduction $ A tax-advantaged health spending account (HSA) gives your employees flexibility in how they save and spend
HSA Contribution Guide How to set up and send employer-directed HSA contributions Introduction $ A tax-advantaged health spending account (HSA) gives your employees flexibility in how they save and spend
Last four digits of the Social Security Number (SSN) match probability increases with submission of a full ID number
 Transaction Facilitator E1 Medicare Eligibility ing Logic Pharmacy Submission Requirements The eligibility inquiry (E1) transaction to the Transaction Facilitator by the pharmacy must include population
Transaction Facilitator E1 Medicare Eligibility ing Logic Pharmacy Submission Requirements The eligibility inquiry (E1) transaction to the Transaction Facilitator by the pharmacy must include population
Affinity Provider Portal - PRISM. User Guide
 Affinity Provider Portal - PRISM User Guide Affinity Medical Group 1221 Broadway, Suite 300 Oakland, California 94612 Affinity Provider Portal - PRISM User Guide Page ii Contents Accessing the Affinity
Affinity Provider Portal - PRISM User Guide Affinity Medical Group 1221 Broadway, Suite 300 Oakland, California 94612 Affinity Provider Portal - PRISM User Guide Page ii Contents Accessing the Affinity
GRADUATE STUDENT EMPLOYEE SELF SERVICE GUIDE
 GRADUATE STUDENT EMPLOYEE SELF SERVICE GUIDE CONTENTS Click any topic below to go directly to that page. HOW TO USE SELF SERVICE 1.1 How to Access, Log In and Navigate Employee Self Service BENEFITS 2.1
GRADUATE STUDENT EMPLOYEE SELF SERVICE GUIDE CONTENTS Click any topic below to go directly to that page. HOW TO USE SELF SERVICE 1.1 How to Access, Log In and Navigate Employee Self Service BENEFITS 2.1
Louisiana Medicaid Management Information System (LMMIS)
 Louisiana Medicaid Management Information System (LMMIS) Electronic Medicaid Eligibility Verification System (emevs Application) User Manual Date Created: 04/13/2004 Date Created: 12/03/2018 Prepared By
Louisiana Medicaid Management Information System (LMMIS) Electronic Medicaid Eligibility Verification System (emevs Application) User Manual Date Created: 04/13/2004 Date Created: 12/03/2018 Prepared By
To access the Bristol Myers-Squibb Expenditures Inquiry, launch your internet browser.
 To access the Bristol Myers-Squibb Expenditures Inquiry, launch your internet browser. In the address field of your browser, type http://supplierlink.bms.com/. In the left navigation bar, under the section
To access the Bristol Myers-Squibb Expenditures Inquiry, launch your internet browser. In the address field of your browser, type http://supplierlink.bms.com/. In the left navigation bar, under the section
Plan Central Employer Portal Learning Guide
 Plan Central Employer Portal Learning Guide Contents Introduction... 2 Enhancements to the New Plan Central... 2 User Roles... 3 Printer Friendly... 3 Accessing Plan Central... 3 Plan Central Welcome Page...
Plan Central Employer Portal Learning Guide Contents Introduction... 2 Enhancements to the New Plan Central... 2 User Roles... 3 Printer Friendly... 3 Accessing Plan Central... 3 Plan Central Welcome Page...
WV MMIS EDI File Exchange User Guide Version 1.0 West Virginia Trading Partner Account Electronic Data Interchange (EDI) File Exchange User Guide
 West Virginia Trading Partner Account Electronic Data Interchange (EDI) File Exchange User Guide Date of Publication: 01/19/2016 Document Version: 1.0 Privacy and Security Rules WV MMIS The Health Insurance
West Virginia Trading Partner Account Electronic Data Interchange (EDI) File Exchange User Guide Date of Publication: 01/19/2016 Document Version: 1.0 Privacy and Security Rules WV MMIS The Health Insurance
Provider Secure Portal User Manual
 Provider Secure Portal User Manual Copyright 2011 Centene Corporation. All rights reserved. Operational Training 2 August 2011 Table of Contents Provider Secure Portal... 5 Registration... 6 Provider -
Provider Secure Portal User Manual Copyright 2011 Centene Corporation. All rights reserved. Operational Training 2 August 2011 Table of Contents Provider Secure Portal... 5 Registration... 6 Provider -
BLUE CROSS AND BLUE SHIELD OF LOUISIANA INSTITUTIONAL CLAIMS COMPANION GUIDE
 BLUE CROSS AND BLUE SHIELD OF LOUISIANA Table of Contents I. Introduction...3 II. General Specifications...4 III. Enveloping Specifications...5 IV. Loop and Data Element Specifications...7 V. Transaction
BLUE CROSS AND BLUE SHIELD OF LOUISIANA Table of Contents I. Introduction...3 II. General Specifications...4 III. Enveloping Specifications...5 IV. Loop and Data Element Specifications...7 V. Transaction
Online Services for Employers User Guide. Mayo Clinic Health Solutions
 Online Services for Employers User Guide Mayo Clinic Health Solutions Table of Contents 1.0 Registering and Signing In... 1 Registration... 1 User Definitions... 1 Signing In... 1 2.0 Enrollment... 3 3.0
Online Services for Employers User Guide Mayo Clinic Health Solutions Table of Contents 1.0 Registering and Signing In... 1 Registration... 1 User Definitions... 1 Signing In... 1 2.0 Enrollment... 3 3.0
Online Claims Submission User Guide
 Online Claims Submission User Guide Important News for Spending Account Participants Flexible Spending Account (FSA) participants can enter claims data through the web and upload images of scanned documentation
Online Claims Submission User Guide Important News for Spending Account Participants Flexible Spending Account (FSA) participants can enter claims data through the web and upload images of scanned documentation
Authorizations Portal
 Authorizations Portal Quick Start Guide 17ED0017 09/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
Authorizations Portal Quick Start Guide 17ED0017 09/16 Blue Cross and Blue Shield of Louisiana is an independent licensee of the Blue Cross and Blue Shield Association and incorporated as Louisiana Health
INSTRUCTIONS TO OBTAIN THE COMPARATIVE EFFECTIVENESS RESEARCH FEE (CERF) CIGNA REPORTING. April 2013
 INSTRUCTIONS TO OBTAIN THE COMPARATIVE EFFECTIVENESS RESEARCH FEE (CERF) CIGNA REPORTING April 2013 CERF AVERAGE COVERED LIFE REPORTS Cigna has created reporting to assist you with the eligibility data
INSTRUCTIONS TO OBTAIN THE COMPARATIVE EFFECTIVENESS RESEARCH FEE (CERF) CIGNA REPORTING April 2013 CERF AVERAGE COVERED LIFE REPORTS Cigna has created reporting to assist you with the eligibility data
VANTAGE TIP SHEET SERIES
 VANTAGE TIP SHEET SERIES Administrator: Organization Setup We recommend using the following workflow when setting up your Organization in Vantage. 1. Confirm organization settings and security permissions
VANTAGE TIP SHEET SERIES Administrator: Organization Setup We recommend using the following workflow when setting up your Organization in Vantage. 1. Confirm organization settings and security permissions
NEW AUTHORIZATION REQUEST USER GUIDE. For Premera Blue Cross Medicare Advantage Plans providers using Clear Coverage
 NEW AUTHORIZATION REQUEST USER GUIDE For Premera Blue Cross Medicare Advantage Plans providers using Clear Coverage 1 CLEAR COVERAGE NEW AUTHORIZATION REQUEST USER GUIDE 1. Log into One Health Port (OHP)
NEW AUTHORIZATION REQUEST USER GUIDE For Premera Blue Cross Medicare Advantage Plans providers using Clear Coverage 1 CLEAR COVERAGE NEW AUTHORIZATION REQUEST USER GUIDE 1. Log into One Health Port (OHP)
Getting Started With IntegratedOTC.com
 Welcome! Getting Started With IntegratedOTC.com If your health plan directed you to IntegratedOTC.com, you may be eligible to get over-thecounter (OTC) items delivered to your home at no cost. You do not
Welcome! Getting Started With IntegratedOTC.com If your health plan directed you to IntegratedOTC.com, you may be eligible to get over-thecounter (OTC) items delivered to your home at no cost. You do not
View my bill online. User guide
 View my bill online User guide View my bill online With View My Bill Online, you can monitor the conferencing charges to your account anytime from anywhere. It s easier than ever to get the charge details
View my bill online User guide View my bill online With View My Bill Online, you can monitor the conferencing charges to your account anytime from anywhere. It s easier than ever to get the charge details
MARTIN S POINT HEALTH CARE PROVIDER PORTAL GUIDE
 MARTIN S POINT HEALTH CARE PROVIDER PORTAL GUIDE The Martin s Point Provider Portal allows registered users to check the status of claims, pre-authorization requests and benefits/eligibility for US Family
MARTIN S POINT HEALTH CARE PROVIDER PORTAL GUIDE The Martin s Point Provider Portal allows registered users to check the status of claims, pre-authorization requests and benefits/eligibility for US Family
When Premera is the secondary payer to Medicare (also known as Crossover
 EDI News December 2007 Adjustments and corrected claims will be added to the Crossover process between Medicare and Premera no later than mid- January 2008. Feature Articles Crossover Adjustment and Corrected
EDI News December 2007 Adjustments and corrected claims will be added to the Crossover process between Medicare and Premera no later than mid- January 2008. Feature Articles Crossover Adjustment and Corrected
IDRP Portal User Guide for Providers and Plans
 IDRP Portal User Guide for Providers and Plans Version 1.0, September 2017 Controlled electronic version prevails over printed copy of this document. Provided by MAXIMUS Federal Services, Folsom, CA. Work
IDRP Portal User Guide for Providers and Plans Version 1.0, September 2017 Controlled electronic version prevails over printed copy of this document. Provided by MAXIMUS Federal Services, Folsom, CA. Work
Web Portal User Guide
 Web Portal User Guide Table of Contents I. Introduction 2 II. User Account 3 III. Accessing Web Portal 5 IV. Eligibility 6 V. Authorization 1. Create Authorization 2. View Authorization 9 20 VI. Claim
Web Portal User Guide Table of Contents I. Introduction 2 II. User Account 3 III. Accessing Web Portal 5 IV. Eligibility 6 V. Authorization 1. Create Authorization 2. View Authorization 9 20 VI. Claim
New York Medicaid Provider Resource Guide
 New York Medicaid Provider Resource Guide Thank you for being a star member of our provider team. WellCare Health Plans, Inc., (WellCare) understands that having access to the right tools can help you
New York Medicaid Provider Resource Guide Thank you for being a star member of our provider team. WellCare Health Plans, Inc., (WellCare) understands that having access to the right tools can help you
The Provider Enrollment Process. Provider Relations BlueCross BlueShield of South Carolina BlueChoice HealthPlan Healthy Blue SM
 The Provider Enrollment Process Provider Relations BlueCross BlueShield of South Carolina BlueChoice HealthPlan Healthy Blue SM Introduction The enrollment process is performed for several reasons: To
The Provider Enrollment Process Provider Relations BlueCross BlueShield of South Carolina BlueChoice HealthPlan Healthy Blue SM Introduction The enrollment process is performed for several reasons: To
